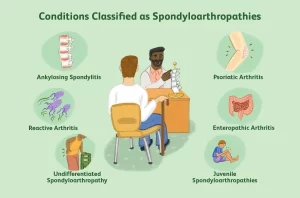
Non-radiographic axial spondyloarthritis, Reactive arthritis, and Enteropathic arthritis
Non-radiographic axial spondyloarthritis is a subgroup created owing to the recognition of early axial disease on MRI. Typically, these patients have symptoms of chronic (often inflammatory) back pain with evidence of (active/acute) sacroiliitis on MRI in the absence of definite X-ray changes. In order to fulfill classification criteria, nr-axSpA patients must also have at least one other SpA features.
Undifferentiated Spondyloarthropathies
Undifferentiated spondyloarthropathy is a syndrome with features consistent with the spondyloarthropathies, but affected patients do not fulfill the criteria for any specific spondyloarthropathy, Undifferentiated spondyloarthropathy may represent an early phase or incomplete form of ankylosing spondylitis or another spondyloarthropathy, However, more recent data suggest that these patients may represent a distinct disease entity.
Reactive arthritis (Reiter’s syndrome)
Reiter’s syndrome (RS) defines a clinical triad of arthritis, conjunctivitis, and urethritis
Specific Infections
Specific infections trigger the clinical features of arthritis (after 3 to 6 weeks) in genetically susceptible patients. These include both chlamydial and mycoplasma urethritis, as well as dysenteric infections caused by salmonella, shigella, and yersinia.
Criteria for diagnosis:
Asymmetric arthritis (mainly peripheral) plus one characteristic extra-articular feature is a sufficient criteria for the diagnosis.
Manifestations
Articular Manifestations
- Asymmetric arthritis: is typically oligoarticular and predominantly in the lower extremities. The most common are knees, ankles, and metatarsophalangeal joints.
- Acute sacroiliitis: May present as a diffuse low back pain that is difficult to localize but may be felt in the deep gluteal area.
- Enthesitis, Plantar fasciitis and Achilles tendinitis: They are quite specific for RS.
Extra-articular Manifestations
- Mucocutaneous: Circinate balanitis (30%).
- Keratoderma Blennorrhagica (20%).
- Painless oral ulcers (25%).
Genitourinary
Urethritis or cervicitis
Gastro-intestinal
Antecedent diarrhea
Ocular
- Uveitis (unilateral) (20%).
- Conjunctivitis (60%).
Psoriatic arthritis
- Chronic inflammatory arthropathy setting of psoriasis.
- Psoriasis is a systemic autoimmune disease.
- Etiology and genotype unclear.
- 5-42% of patients with psoriasis will develop psoriatic arthritis (skin usually precedes joints).
- The frequency of PSA increases with disease severity and duration.
- Nail changes: pitting, dystrophy, onycholysis.
- Course: chronic, destructive arthritis in 30-50%.
Types
- Asymmetrical oligo-arthritis (Most common): Morning stiffness, DIP and PIP involvement, nail disease, ≤ 4 joints involved, Incidence is 40%.
- Symmetric polyarthritis: Symmetric polyarthritis, RA-like distribution, but RF negative, Incidence is 25%.
- Axial spondylitis: Inflammatory low back pain, sacroiliitis, axial involvement, 50% HLA-B27+, Incidence is 20%.
- Distal interphalangeal joint disease: Nail changes often bilateral joint involvement, Incidence is 15%.
- Arthritis mutilans: Destructive form of arthritis, telescoping digits, joint lysis, typically in phalanges metacarpals, Incidence is <5%.
Enteropathic arthritis
Enteropathic arthritis can be defined as arthritis induced by or occurring with intestinal disease, IBS (ulcerative colitis and Crohn’s disease), Whipple’s disease, & post-enteritic reactive arthritis
Axial arthritis (sacroiliitis and spondylitis):
- More common in Crohn’s disease (CD) than in ulcerative colitis (UC).
- Independent of GI symptoms.
Peripheral arthritis:
- Non-deforming and non-erosive.
- May precede intestinal involvement, but usually concomitant or subsequent to bowel disease, as late as 10 years following the diagnosis.
Juvenile ankylosing
Arthritis and enthesitis, or arthritis or enthesitis with at least two of the following:
- Sacroiliac tenderness and/or inflammatory with morning stiffness, improves on movement) lumbosacral pain (at rest).
- The presence of HLA-B27 antigen.
- The onset of arthritis in a male over six years of age.
- Acute (symptomatic) anterior uveitis.
- History of ankylosing spondylitis, enthesitis-related arthritis, sacroiliitis with inflammatory bowel disease, Reiter’s syndrome, or acute anterior uveitis in a first-degree relatives.
Affects males more than females at ages more than 8 years.
Acute Anterior uveitis
- Idiopathic Anterior uveitis.
- There is HLA B27 positivity in 50% of cases.
- Characterize by being recurrent and Unilateral > bilateral.
ASAS classification criteria of SpA
- AS, without treatment or with delayed treatment, is associated with symptomatic burden and loss of function during years that are normally productive.
- An average delay of 8-11 years between onset of symptoms and time of diagnosis has been reported.
The reasons for the delay in diagnosis are:
- Lack of a pathognomonic clinical feature or laboratory test.
- Low back pain is extremely common in the general population, and often the inflammatory origins of back pain are not carefully sought in practice.
- Radiographic sacroiliitis, which has been a cornerstone of diagnosing AS (New York criteria), may take several years to develop.
A substantial improvement in the early diagnosis of AS and the whole group of SpA has occurred in the last decade due to:
- Introduction of MRI as one of the key diagnostic tools in detecting the earliest signs of inflammation (early diagnosis leads to early initiation of effective treatment and improves outcome).
- Development of new classification criteria SpA.
Axial SpA (axSpA) encompasses patients with inflammation of the axial skeleton. axSpA includes patients with AS with established sacroiliitis on X-ray. It also includes a further subgroup called non-radiographic axial SpA (nr-axSpA). pSpA refers to disease with predominantly peripheral features of enthesitis, arthritis, or dactylitis.
Significant advances have been made in the treatment of axSpA, Despite the efficacy of biologics, NSAIDs continue to be the first-line treatment for patients with axSpA, and non-pharmacological treatment modalities continue to be important in the management of these patients.
For the first time in many years, a new therapeutic approach has been approved (Targeting IL-17) and others show promise in axSpA, The introduction of BIOSIMILARS has greatly reduced the cost associated with biologic treatment, Trying to establish which patient benefits the most from each drug is a challenge for the future.
You can subscribe to Science Online on YouTube from this link: Science Online
You can download the Science Online application on Google Play from this link: Science Online Apps on Google Play
Rheumatoid Arthritis (RA) causes, stages, symptoms, diagnosis, and specific joint affection
Rheumatoid Arthritis diagnosis and treatment, Disease-Modifying antirheumatic drugs (DMARDs)