Pelvic peritoneum, Muscles of the pelvic wall, Pelvic vessels, Sacral plexus branches
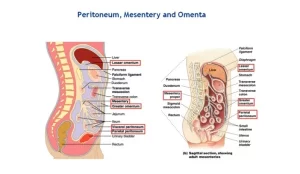
Pelvic peritoneum covers most of the intra-abdominal (or coelomic) organs, It is composed of a layer of mesothelium supported by a thin layer of connective tissue, It is the serous membrane forming the lining of the abdominal cavity or coelom in amniotes and some invertebrates, such as annelids, It is the inferior reflection of the peritoneum over the fundus of the urinary bladder and the front of the rectum at the junction of its middle and lower thirds.
Pelvic peritoneum
In Male: The peritoneum lining the lower part of the abdominal wall is reflected backwards to cover the superior surface than the upper part of the posterior surfaces of the bladder. Then, it passes backwards above the seminal vesicle to cover the front of the middle third of the rectum to form a rectovesical pouch (7.5 cm above the anal orifice). Then it passes upwards to cover the front and sides of the rectum.
In Female: The peritoneum is reflected from the lower part of the anterior abdominal wall to cover the upper surface of the urinary bladder. Then it is reflected on the front of the uterus at the junction between the body and cervix to form uterovesical pouch, then it covers anterior surface of the body of the uterus, fundus of the uterus, posterior surface of body and cervix of the uterus, and upper part of the posterior wall of the vagina (posterior fornix).
Then the peritoneum reflects on front of the middle third of the rectum to form a recto-uterine pouch (Douglas pouch) (5.5 cm above the anal orifice). The peritoneum covering the sides of the uterus, is reflected laterally onto the side of the pelvis to form the broad ligament.
Applied anatomy: Collection in Douglas poutch could be drained by puncture of the posterior fornex of the vagina.
Pelvic wall
Muscles of the pelvic wall:
- Piriformis.
- Obturator internus.
Piriformis muscle
- Origin: pelvic surface of middle 3 sacral pieces.
- Insertion: top of greater trochanter of the femur.
- Nerve supply: S1 S2 (from the sacral plexus).
- Action: lateral rotation of the thigh.
Obturator internus
- Origin: the inner surface of obturator membrane Inner surface of ilium, below the arcuate line.
- Insertion: medial side of greater trochanter of the femur.
- Nerve supply: nerve to obturator internus.
- Action: lateral rotation of the thigh.
Obturator fascia
The Obturator fascia covers the pelvic surface of the obturator internus, It is thickened in its upper part forming what is called a tendinous arch= white line, The tendinous arch gives attachment to the levator ani muscle.
Pelvic floor
It consists of a gutter-shaped sheet of muscle (pelvic diaphragm), surrounding the midline passages (urethra, vagina, analcanal).
Muscles of the pelvic floor
- Levator ani.
- Coccygeus.
Levator ani muscle
It is an abroad muscle that arises from the side of the lesser pelvis and unites with its fellow of the opposite side to form the greater part of the pelvic floor.
Origin: it arises from a line extending from the pelvic surface of the body of the pubis, a white line of obturator fascia (tendinous arch), and the inner surface of the ischial spine.
Insertion: as the fibers pass backwards, it can be differentiated into 3 parts:
- Pubococcygeus: inserted into perineal body & tip of coccyx, fibers of this part pass across the side of the prostate in male (levator prostate) and across the side of vagina (sphincter vagina) in female.
- Ilíococcygeus: inserted into the sides of the last 2 pieces of the coccyx and anococcygeal raphe which extends from the apex of the coccyx to the anorectal junction.
- Puborectalis: passes backwards, at anorectal junction, fibers of both sides, It forms a U-shaped sling which helps the deep part of the external anal sphincter.
Minor parts of levator ani
They all form sling-like action around tubular structures.
- Levator prostate: It is a U-shaped sling of muscle fibers that passes behind the prostate.
- Pubo-vaginalis (sphincter vaginae): It is a U-shaped sling of muscle fibers that passes behind the vagina.
- Pubo-uretheralis: It is another U-shaped sling of muscle fibers that passes behind the urethra.
Nerve supply: Ventral rami of S3, 4 sacral nerve and inferior rectal nerve.
Action of levator ani
- Acting together both muscles increase the intra-abdominal pressure so, it helps in defecation and labour.
- Puborectalis, supports external anal sphincter
- Pubococcygeus: supports the prostate in male and acts as a sphincter for the vagina.
Clinical note: during labour, the perineal body may be torn leading to prolapse of the uterus because the gap between the anterior border of the 2 levator ani becomes wider.
Coccygeus muscle
- It is a small muscle that lies behind the levator ani and forms part of the pelvic floor.
- Origin: the tip of the ischial spine.
- Insertion: sides of the last 2 sacral pieces and 1st coccygeal piece.
Pelvic vessels
Internal iliac artery
- Origin: It is the smaller one of the 2 terminal branches of the common iliac artery.
- Course: It begins at the level of the lumbosacral angle opposite to the sacroiliac joint. It passes backwards and downwards.
- It ends by division into anterior and posterior division near the upper border of greater sciatic foramina.
Branches of the anterior division
A) Parietal branches:
- Obturator artery.
- Inferior gluteal artery.
- Internal pudendal artery.
B) Visceral branches:
- Umbilical artery and its superior vesical branch.
- Inferior vesical artery (in male) (replaced by a vaginal artery in female).
- Uterine artery (in female).
- Middle rectal artery.
Branches of the posterior division
- Iliolumbar artery.
- Two lateral sacral arteries.
- Superior gluteal artery.
Median sacral artery
- Origin: the back of the abdominal aorta just above its bifurcation.
- Course & relations: It descends in the midline, in front of L4,5 vertebrae and the sacral promontory, and the concavity of the sacrum behind the rectum.
- Termination: it ends by the formation of a swelling called Glomus coccygeum in front of the coccyx.
Branches:
- Last pair of the lumbar arteries (5th lumbar).
- Small branches to the sacral canal.
- Small branches to the rectum.
Embryologically, this artery represents the continuation of the aorta.
Internal iliac vein
It is the main vein draining the pelvis. It is formed by the union of most of the veins which accompany the branches of the internal iliac artery just above the greater sciatic foramen. It receives the following tributaries:
- Superior gluteal V.
- Lateral sacral Vs.
- Obturator V.
- Middle rectal V.
- Vesical Vs.
- Uterine V. in ♀.
- Vaginal V. in ♀.
- Int. pudendal V.
- Inferior gluteal V.
The visceral tributaries of the internal iliac vein arise from the venous plexuses around or in the walls of the viscera. These are:
- Vesical venous plexus.
- Prostatic venous plexus.
- Uterine venous plexus.
- Vaginal venous plexus.
- Rectal venous plexuses.
Median sacral vein
It closely accompanies the artery and ends in the left common iliac vein.
Superior rectal vein
It ascends close to the left side of the artery and continues up as the inferior mesenteric vein.
Sacral plexus
Definition & formation: It is a flat triangular structure formed by the ventral rami of L4,5 (lumbosacral trunk) and S1,2,3,4. Ventral rami of L4 and L5 form the lumbosacral trunk, this trunk will emerge from the medial margin of the psoas major to join the 1st sacral nerve anterior to the sacroiliac joint.
Site: on the posterior pelvic wall, in front of the piriformis and behind the parietal pelvic fascia, sigmoid colon, and rectum.
Branches
(A) From the roots of the plexus
Ventral branches:
- Pudendal nerve (S2,3,4).
- The pelvic splanchnic nerve (S2,3,4), gives the parasympathetic supply to pelvic organs.
- Perineal branch of S4 (supply external anals sphincter).
Dorsal branches
4. Nerve to Piriformis (S1,2)
5. Posterior cutaneous nerve of the thigh (S1,2,3).
6. Perforating cutaneous nerve (S2,3).
(B) From the plexus itself
Ventral branches:
- Nerve to quadrates femoris (L4,5-S1).
- Nerve to obturator internus (L5-S1,2).
- Tibial part of the sciatic nerve (L4,5-S1,2,3).
Dorsal branches:
4- Superior gluteal nerve (L4,5-S1).
5- Inferior gluteal nerve (L5-S1,2).
6- Common peroneal part of the sciatic nerve (L4.5-S1,2).
7- Two terminal branches are the pudendal & sciatic nerves.
You can follow science online on YouTube from this link: Science online
You can download Science Online application on Google Play from this link: Science online Apps on Google Play
Bony pelvis structure, types, organs, Differences between male & female pelvis
Divisions of Perineum, Fascia of Urogenital triangle & Contents of Ischiorectal fossa