Ventilation-perfusion relationships and why is ventilation higher at the base of the lung
The function of respiration is to keep blood gases at a normal level through a balance between 2 main mechanisms: ventilation and perfusion. Under normal resting conditions, alveolar ventilation and pulmonary blood flow are approximately equal; average resting alveolar ventilation is about 4 L/min and average pulmonary blood flow is about 5 L/min, the normal ratio being 0.8.
Ventilation-perfusion relationships
At rest, a large part of the lung remains inactive. Only on exercise do we both ventilate and perfuse the entire lung. With the lung in only partial use most of the time, it follows that individual gas exchange units may be in different states of activity. The following types of units may be recognized:
- Normal unit both ventilated & perfused.
- Dead space unit ventilated, poorly, or non-perfused.
- Shunt unit perfused, poorly, or non-ventilated.
So we can conclude that a slight ventilation-perfusion imbalance exists in healthy persons. Moreover, increased (above normal) mismatching of ventilation and perfusion is by far the most common cause of arterial hypoxia in lung diseases.
Effect of alterations of the ventilation-perfusion ratio on the Po2 and Pco2 in a lung unit
- The unit in the center receives ventilation and blood flow in ideal proportions, therefore the alveolar O₂ tension is about 100 mm Hg and alveolar CO₂ tension 40 mm Hg. The blood leaving this unit would have the same gas tensions as found in the alveoli
- The unit on the left receives no ventilation i.e. alveoli perfused but not ventilated. Therefore, its VIQ ratio equals zero. The blood leaving the unit has the same mixed venous Po2 and Poc2 as that entering i.e. behaves as a shunt.
- The unit on the right, receives no blood flow i.e. alveoli are ventilated but not perfused. Here the ventilation is called wasted ventilation (i.e. alveolar dead space and therefore has a V/Q ratio of infinity (∞).
Regional V/Q in the normal lung
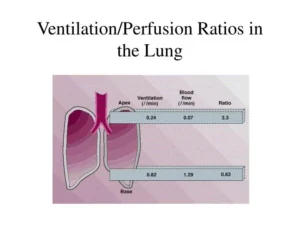
Ventilation increases slowly from top to bottom of the lung. Blood flow increases more rapidly from the top to the bottom of the lung. The lung at the apex is more ventilated than perfused (high V/Q ratio units), while the lung at the base is more perfused than ventilated (low ratio units).
As a consequence, the V/Q ratio is abnormally high at the top of the lung (where the blood flow is minimal) and much lower at the bottom. V/Q Ratio at the apex of the lung-3.3. V/Q Ratio at the base of the lung 0.6.
Diffusion
After the alveoli are ventilated with fresh air, the next step in the respiratory process is the transfer of gases across the blood-gas barrier. Diffusion is the exchange between alveolar and blood gases (O₂ and CO₂) through the alveolo-capillary membrane.
Diffusion through tissues is described by Fick’s law which states that: The rate of diffusion of a substance through a membrane is directly proportional to the surface area of the membrane, the solubility of the substance in the membrane and the pressure gradient. It is inversely proportional to the thickness of the membrane and the square root of the molecular weight.
Factors affecting the rate of diffusion through the respiratory membrane
1. Thickness of the membrane: The overall thickness of the membrane is about 0.5 micron. The rate of diffusion of gases is inversely proportional to the thickness of the respiratory membrane. Increased thickness (as in pulmonary fibrosis, congestion or oedema) decreases diffusion.
2. Surface area of the membrane: The surface area of the respiratory membrane is very large about 50-100 sq meters (70m²) in the normal adult. The surface area is decreased in the removal of one lung in emphysema many of the alveoli coalesce, with the dissolution of many alveolar walls. Therefore, the new chambers are much larger than the original alveoli, but the total surface area is often decreased because of the loss of alveolar walls.
3. Pressure gradient: The pressure gradient across the respiratory membrane is the difference between the partial pressure of the gas in the alveoli and its partial pressure in the blood (pulmonary capillaries).
The pressure of O₂ in the alveoli (100 mm Hg) is greater than its pressure in the venous blood entering the pulmonary capillaries (40 mm Hg). Therefore, O₂ diffuses from alveoli to the blood.
The pressure of CO₂ in the blood entering the pulmonary capillaries (46 mm Hg) is greater than its partial pressure in the alveoli (40 mm Hg). Therefore, CO₂) diffuses from the blood into the alveoli.
4. The diffusion coefficient for the transfer of each gas through the respiratory membrane depends on its solubility in the membrane and the square root of its molecular weight. The greater the solubility of the gas, the greater will be the number of molecules available to diffuse for any given pressure difference. CO₂ is more than 20 times as soluble as oxygen in the tissue water.
Diffusion capacity of the respiratory membrane
It is the volume of a gas that diffuses through the membrane each minute with a pressure difference of 1mmHg. It is expressed in ml/ min/ mm Hg. All factors discussed above that affect diffusion through the respiratory membrane can affect the diffusing capacity.
Diffusion capacity for O2
It increases during exercise by several factors, among which are:
- Opening up of a number of previously dormant pulmonary capillaries (recruitment) or dilation of already open capillaries (distension), thereby increasing the surface area of the blood into which the oxygen can diffuse.
- A better match between the ventilation of the alveoli and the perfusion of the alveolar capillaries with blood. Therefore, during exercise, the oxygenation of the blood is increased not only by increased alveolar ventilation but also by a greater capacity of the respiratory membrane for transmitting oxygen into the blood.
Equilibration for Oxygen
Normally enough O₂ diffuses across the respiratory membrane so that the blood O₂ tension and the alveolar O₂ tension equalize in about 0.25 second (Equilibration time). In normal lungs, blood travels along pulmonary capillaries in about 0.75 second (Transit time).
The blood normally stays in lung capillaries about 3 times as long as necessary to cause full oxygenation. Therefore, there is about 0.5 sec with no increase in O₂ content. This time provides a safety margin or reserve that ensures adequate O₂ uptake during periods of stress e.g. exercise and diffusion defects as thickening of respiratory membrane.
In exercise, the blood travels along pulmonary capillaries in about 0.25 second. Therefore, there is complete oxygenation of blood in this rapid time.
Oxygen transport by blood, Importance of P50, Bohr Effect and Treatment of CO poisoning
Regional differences in ventilation, Pulmonary circulation, Shunt and Lung perfusion zones
Mechanics of ventilation, Structures of Respiratory system and Functions of conducting zone
Mechanics of Pulmonary Ventilation and Pressure changes during Respiratory cycle
Normal and abnormal lung compliance, Elastance, Surfactant and work of breathing