Normal and abnormal lung compliance, Elastance, Surfactant and work of breathing
Pulmonary compliance is a measure of lung expandability. It is important for ideal respiratory system function. It refers to the ability of the lungs to stretch and expand. Compliance of the respiratory system describes the expandability of the lungs and chest wall. There are two types of compliance: dynamic and static.
Lung compliance
The compliance of the lung describes the relationship between the transmural pressure (ie pressure passing through a wall eg hollow structure) across the lung compared with the organ’s volume. Compliance is the extent to which the lungs expand for each unit increase in transpulmonary pressure.
C = ΔV/ ΔP = Change in lung volume/change in transpulmonary pressure
Transpulmonary pressure is the pressure difference between the alveolar pressure and the pleural pressure. When the glottis is open, and no air is flowing into or out of the lungs, the pressures in all parts of the respiratory tree (all the way to the alveoli) are all equal to atmospheric pressure, which is considered to be 0 cm H2O pressure.
PA = zero ∴ C = ΔV/ ΔIPP = ml/ cm H2O
Elastance
Compliance reflects distensibility. The reciprocal of the compliance is the elastance i.e elastic recoil pressure. When the lungs are remarkably distensible, this means that their compliance is high while their elasticity is low.
Elastance = 1/complicance
Normal value of compliance
Total compliance (Compliance of the lungs & thoracic cage) = 130 ml/cm H₂O pressure. This means that every time the pleural pressure decreases by 1 cm H₂O, the lungs and thoracic cage expand 130 ml. In other words, every time the negativity of the pleural pressure increases by 1cm H₂O, the lungs and thoracic cage expand 130 m. Compliance of the lungs alone = 200 ml/cm H₂O pressure.
The lung alone has higher compliance than the total compliance because the chest wall movements are limited by the bony wall and respiratory muscles ie. the inspiratory muscles must use energy not only to expand the lungs but also to expand the thoracic cage around the lungs.
Abnormal compliance
Reduced compliance
- Rigid lung e.g. fibrosis, congestion, and pulmonary oedema.
- Rigid thoracic cage e.g. deformities of the vertebral column, such as kyphosis (posterior bending) and scoliosis (lateral bending), limit expansion of the lungs and extensive burns to the thorax.
Increased compliance
- Old age.
- Chronic obstructive pulmonary (COPD) [Emphysema+ Chronic bronchitis].
Emphysema is an abnormal permanent enlargement or dilatation of the air spaces distal to the terminal bronchioles, accompanied by destruction of their walls. Males are more affected than females, especially heavy smokers.
Chronic bronchitis is caused by chronic irritation by heavy cigarette smoking. This chronic irritation stimulates hypersecretion of mucous and hypertrophy of mucous glands in the trachea and bronchi. Microbic infection is important in maintaining inflammation and may cause acute exacerbation.
Surfactant and work of breathing
Surfactant
Surfactant is a surface tension-lowering agent. It is produced by type II alveolar epithelial cells as lamellar bodies (membrane-bound organelles containing whorls of phospholipid) and secreted into the alveolar lumen by exocytosis. Surfactant is a mixture of phospholipids, mainly dipalmitoyl phosphatidyl-choline (DPPC), other lipids, and proteins. Excess surfactant is removed by pulmonary alveolar macrophages and by endocytosis into type Il cells.
Mechanism of action of surfactant
Surfactant particles spread as a monomolecular layer at the interface between air and fluid lining the alveoli. Each phospholipid molecule has a hydrophilic head and a hydrophobic tail. The hydrophilic head dissolves in water, lining the alveoli whereas, the hydrophobic tail is oriented towards alveolar air and doesn’t dissolve in the fluid. It scatters among the fluid molecules, decreasing the attraction between them or repelling surface molecules of the fluid away from each other therefore lowering the surface tension.
Physiological significances of surfactant
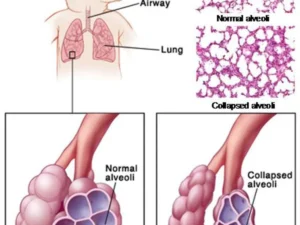
- Decreasing the surface tension: It minimizes the effect of the high surface tension of the fluid lining the alveoli and prevents the collapse of the lung. The decrease in surface tension increases lung compliance and reduces the work needed for expansion with each breath.
- Stability of the pulmonary alveoli: It is very important in maintaining the pressure inside them.
- It helps to keep the alveoli dry: Surfactant prevents transudation of fluid in the alveoli by reducing surface forces which tend to suck fluid into the alveolar spaces from the capillaries (prevent the development of pulmonary oedema).
- Surfactant keeps the lungs from collapsing after expansion at birth. The fetal lung is not collapsed but is inflated with liquid to about 40% of its total capacity. This fluid is continuously secreted by alveolar cells during fetal life. Some of it is squeezed out as the infant moves through the birth canal, and some is removed by lymphatics and capillaries. The remainder has an important role in the subsequent inflation of the lung.
Infant respiratory distress syndrome (IRDS)
Type Il cells of the lung, which form surfactant, first appear in the human fetus at about 20 weeks of pregnancy, and surfactant secretion is established by 30 weeks. If the Infant is born before that time, he may have a surfactant deficiency, which can cause infant respiratory distress syndrome.
Lung expansion is extremely difficult in the absence of surfactant; it often requires very high negative intrapleural pressure to overcome the collapse tendency of the alveoli. The surface tension in the lungs of these infants is high with areas of atelectasis (collapsed alveoli), and alveoli are filled with fluid.
Acute respiratory distress syndrome (ARDS)
Cigarette smoking is harmful because smoke increases alveolar macrophage activity, which increasesthe removal or decreases the secretion of surfactants.
Factors affecting the formation of surfactant
Factors that stimulate its formation are:
- Thyroid hormones.
- Glucocorticoid hormones.
Factors that decrease the formation of surfactants are:
- Insulin hormone inhibits surfactant apoproteins formation.
- Long-term inhalation of pure O2.
- Cessation of pulmonary circulation for a long time.
Work of breathing
The respiratory muscles normally perform “work” only to cause inspiration and not to cause expiration. Expiration is almost entirely a passive process caused by the elastic recoil of the lung and chest cage structures. The work of inspiration can be divided into three fractions:
- Compliance work or elastic work: This is the work required to expand the lungs against the lung and chest elastic forces. The elastic resistance accounts for 65% of the overall resistance to ventilation.
- Airway resistance work: This is the work required to overcome airway resistance during the movement of air into the lungs. The tissue airway resistance accounts for 28% of the overall resistance to ventilation.
- Tissue resistance work: This is the work required to overcome the viscosity of the lung and chest wall structures. The resistance accounts for 7% of the overall resistance to ventilation. The airway resistance and tissue resistance represent the nonelastic resistance to ventilation. They account for 80% and 20% of all nonelastic resistance, respectively.
In pulmonary disease, all three types of work are frequently vastly increased. Compliance work and tissue resistance work are especially increased by diseases that cause fibrosis of the lungs, and airway resistance work is especially increased by diseases that obstruct the airways.
During normal quiet respiration, no muscle “work” is performed during expiration because expiration results from the elastic recoil of the lungs and chest. In heavy breathing or when airway resistance and tissue resistance are great, expiratory work does occur and sometimes becomes even greater than inspiratory work. This is especially true in asthma, which often increases airway resistance many folds during expiration but much less so during inspiration.
You can follow Science online on YouTube from this link: Science online
Mechanics of Pulmonary Ventilation and Pressure changes during Respiratory cycle
Diaphragm anatomy, structure, function, Phrenic nerves and Nerves of the thorax
Lung structure, borders, Lobes, Fissures and Broncho-pulmonary segments
Trachea, Major Bronchi, Thoracic cavity structure, function and anatomy
Larynx structure, function, cartilages, muscles, blood supply and vocal folds