Nystagmus types, causes, symptoms Development of CNS and Abnormalities of Spinal cord
Nystagmus is a repetitive rhythmic slow movement of the eyes to one side followed by a fast movement of the eyes in the opposite direction. It was observed at the start of rotation for about 30 seconds (rotatory nystagmus and at the end of a period of rotation for 30 seconds (post rotatory nystagmus).
Components of rotatory nystagmus
- Slow component: The slow component is the vestibulo-ocular reflex which aims to maintain visual fixation.
- Rapid component: rapid jumping of both eyes in the same direction of rotation. The rapid component is generated by the reticular formation in the brainstem which discharges to the nuclei of the Ill and VI cranial nerves through the medial longitudinal bundle producing rapid jumping of both eyes in the same direction of rotation. Thus the slow component is controlled by signals from the vestibular apparatus (vestibulo-ocular reflex) and the rapid component is controlled by brainstem circuits (reticular reflex).
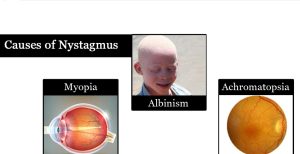
Causes of nystagmus
Physiological causes of nystagmus:
- Angular acceleration (Rotation).
- Looking from the window of a rapidly moving car (optokinetic nystagmus).
Pathological causes of nystagmus:
- Lesions of the labyrinth vestibular nerve or nuclei.
- Cerebellar diseases.
Development of CNS
Origin: ectoderm
Development:
- At the 3rd week, an ectodermal thickness (neural plate) appeared in the mid-dorsal region cranial to the primitive node.
- The lateral edges of this plate are called the neural folds.
- These folds elevate and approach each other in the midline. They fuse together to form the neural tube.
- The neural tube is separated from the surface ectoderm. The fusion occurs at the 4th week; it starts in the cervical region and extends cranial and caudal.
- Once fusion is initiated the opened end of the neural tube form cranial and caudal neuropores which are communicated to the amniotic cavity.
The cranial portion of the neural tube shows 3 dilatations:
- Prosencephalon: (forebrain vesicle). In the 5th week, it differentiates into a central portion called diencephalon having the optic vesicle, and 2 lateral extensions called the telencephalon.
- Mesencephalon (midbrain vesicle).
- Rhombencephalon (hindbrain vesicle). This differentiates into metencephalon (future pons and cerebellum) and myelencephalon (future medulla oblongata.
2 flexures appear:
- Cephalic flexure: in the midbrain region.
- Cervical flexure: at the junction between the hindbrain and spinal cord.
Later on, another flexure called pontine flexure appears between the pons and myelencephalon.
The neural canal (cavity of the neural tube):
- The cavity in the telencephalon forms the lateral ventricle.
- The cavity in the diencephalon forms the 3rd ventricle.
- The cavity of the hindbrain forms the 4 ventricles.
- The cavity in the spinal cord forms the central canal.
Neural crest cells
This is a group of calls on either side of the neural plate. They originate from ectoderm. They are found along the whole length of the neural tube. The cells of the neural crest migrate to form neural crest derivatives.
- Melanocytes.
- Meninges (pia & arachnoid matter).
- The mesenchyme of the pharyngeal arches.
- Suprarenal medulla.
- Schwann cells (neurilemmal sheath of peripheral nerves).
- Ganglia (spinal & autonomic).
- Ganglion cell layer of the retina.
- Odontoblasts.
- Carotid body.
Development of the spinal cord
Origin: from the caudal part of the neural tube.
Development:
- The neuroepithelial cells lined the caudal part of the neural tube proliferate to form neuroblastic cells. These cells accumulate superficial to the neuroepithelial lining of the tube.
- They form the mantle layer (future grey matter).
- The proliferation of the mantle cells leads to the formation of the marginal layer, this layer lies superficial to the mantle layer. Myelination of the nerve fibers of the marginal layer leads to the formation of the white matter of the spinal cord.
- The additional thickness of the neuroblasts of the mantle layer leads to the formation of dorsal & ventral thickness in the mantle layer.
- The dorsal thickness is a sensory area (alar plate or lamina=future dorsal sensory horn). The ventral thickness is a motor area and called basal plate or lamina (future motor horn).
- The 2 plates are separated on the surface by sulcus limitans.
- The 2 alar plates are separated by the roof plate that lies in the dorsal midline.
- The floor plate that lies in the ventral midline separates the two basal plates. The roof & floor plates are devoid of neuroblasts; they are pathways for the crossing of nerve fiber from side to the other.
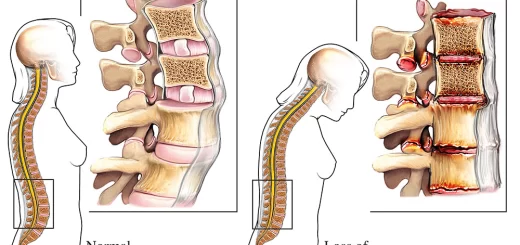
Abnormalities of the spinal cord
Neural tube defect (spina bifida): This anomaly is due to abnormal closure of the neural folds which is normally occurred at the 3rd or 4th week. In this defect, there is a splitting of vertebral arches, which may be accompanied by the splitting of the underlying neural tissue. There are 2 types of spina bifida:
a. Spina bifida occulta: There is a defect of the vertebral arch covered with a patch of hair a. Spina overlying the lesion. The neural tissue is normal). It occurs in the lumbosacral region.
b. Spina bifida cystica: There are defects of the vertebral arch & severe neural tube defects affecting the neural tissue and/or meninges. The neural tissue and/or meninges protrude through the defect in the skin and the vertebral arch. It occurs in the lumbosacral region. This condition is not associated with mental retardation. There are 3 types:
- Meningocele: defect in the vertebral arch and swelling of meninges (Meningeal sac containing CSF).
- Meningomyelocele: meningocele + meningeal sac containing the herniated spinal cord.
- Syringomyelocele: meningomyelocele + dilatation of the neural canal.
Development of medulla oblongata
It develops from the myelencephalon. The roof plate extends and is covered with the vascular pia mater. The roof plate is formed by a single layer of ependymal cells covered with the vascular pia matter forming the tela choroidae. As a result of the extension of the roof plate, the alar lamina becomes lateral to the basal lamina, Both laminae are separated by the sulcus limitans.
Both laminae contain nuclei arranged in columns:
A. The basal lamina (motor): contains three different columns. These columns are arranged from medial to lateral;
- GSE column: contains cranial nerve nuclei motor to skeletal muscles (derived from somite).
- SVE column: contains cranial nerve nuclei motor to striated muscles derived from branchial arches.
- GVE column: contains cranial nerve nuclei motor to smooth muscles of the thoracic and abdominal viscera (parasympathetic column).
B. The alar lamina (sensory): contains four different columns. These columns are arranged. from medial to lateral;
- GVA column: contains cranial nerve nuclei receiving sensory fibers from thoracic and abdominal viscera.
- SVA column contains cranial nerve nuclei receiving sensory fibers from the tongue, palate, and oropharynx.
- GSA column: contains cranial nerve nuclei receiving sensory fibers from the skin of the head.
- SSA column: contains cranial nerves nuclei related to hearing and equilibrium.
You can subscribe to Science Online on YouTube from this link: Science Online
You can download the Science Online application on Google Play from this link: Science Online Apps on Google Play
Visual pathway, functions of neurons in Primary visual cortex & Analysis of visual information
Retinal receptors, Photochemistry of vision, Steps of phototransduction in rods & Retinal output
Sense of vision, Refractive media of the eye, Corneal reflex & Pupillary pathways
Retina function, anatomy, layers, and accessory structures of the eye
Eyes structure, Histological organization of the fibrous and vascular coast of the eye
Visual system, Bony orbit anatomy, contents & Nerves, Muscles & movements of Eyeball