Vas deferens function, histology, anatomy, Varicocele and Functions of Seminal vesicle
Vas deferens is a thick-walled cord-like duct, it has a very narrow lumen. It is 30-45cm in length. Beginning: at the lower end of the tail of the epididymis. It ascends along the posterior border of the testis, medial to the epididymis. It runs up in the posterior part of the spermatic cord, where it is surrounded by the pampiniform venous plexus.
Vas deferens
Vas deferens enters the inguinal canal, within the spermatic cord. It enters the pelvis by passing through the deep inguinal ring, here it curves lateral to the inferior epigastric artery. It descends along the lateral pelvic wall crossing obturator vessels and nerves, obliterated umbilical artery, and external iliac vessels. Close to the base of the urinary bladder, it crosses the front of the terminal part of the ureter.
It presents a dilated ampulla which lies medial to the seminal vesicle behind the base of the urinary bladder. At the base of the prostate, it narrowens and joins the duct of the seminal vesicle to form the ejaculatory duct. Arterial supply: artery of vas, which arises from the superior or inferior vesical artery.
In the histological section: Vas deferens has an irregular lumen with longitudinal folds, The wall is formed of 3 concentric coats:
- Mucosa: lined by pseudostratified columnar epithelium with stereocilia. The lamina propria is rich in elastic fibers.
- Musculosa: consists of 3 densely-packed layers of smooth muscle fibers, thin inner longitudinal layer, thick middle circular layer, and a moderately thick outer longitudinal layer.
- Adventitia: formed of loose connective tissue.
The function of vas deferens: the musculosa produces strong peristaltic contractions during ejaculation, which rapidly move sperms from the epididymis along the vas into the ejaculatory duct.
In histological sections, vas deferens is seen together with other structures forming the coverings and contents of the spermatic cord.
Spermatic cord
Site: Spermatic cord is formed at the deep inguinal ring and passes through the inguinal canal to enter the scrotum, where it is attached to the testis.
Coverings:
- Internal spermatic fascia (innermost coat): is derived from fascia transversalis.
- Cremasteric muscle and fascia (the middle coat): derived from the internal oblique muscle.
- External spermatic fascia (the outer coat): derived from aponeurosis of the external oblique muscle.
Contents:
- Vas deferens
- Artery of the vas: a branch of the inferior vesical artery.
- Cremasteric artery: a branch of the inferior epigastric artery.
- Testicular artery: a branch of the abdominal aorta.
- Pampiniform venous plexus: ends at the deep inguinal ring to form the testicular vein.
- Sympathetic fibers.
- Genital branch of genitofemoral nerve: it supplies the cremasteric muscle.
- Lymphatic vessels: which drain the testis and ascend to the para-aortic lymph nodes.
- Vestigue of processus vaginalis (obliterated processus vaginalis).
Clinical notes
Varicocele is a condition in which the veins of the pampiniform plexus are elongated and dilated. It is a common disorder in adolescents and young adults, with most occurring on the left side. This is thought to be because the left testicular vein joins the left renal vein at the right angle, the left testis is slightly lower than the right one, and the pressure of the sigmoid colon on the left testicular vein.
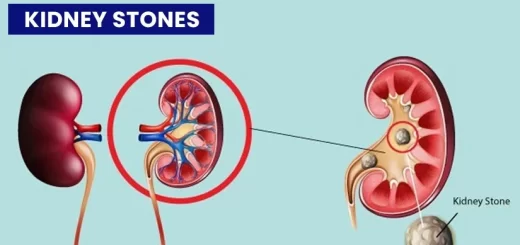
Rarely, malignant disease of the left kidney extends along the renal vein and blocks the exit of the testicular vein A rapidly developing left-sided varicocele should therefore always lead one to examine the left kidney.
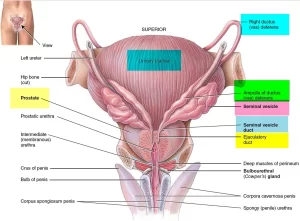
Seminal vesicle
There are 2 large, sacculated pouches about 5 cm long. It contains a tubule 15 cm long.
Site: on the base of the urinary bladder, anterior to the rectum, and lateral to the vas deferens. Its lower end joins the vas deferens to form the ejaculatory duct.
Arterial supply: inferior vesical and middle rectal arteries.
In the histological section: the seminal vesicle appears formed of a number of cut sections with isolated lumina. The wall consists of 3 layers.
- Mucosa: Extremely folded and thrown into primary, secondary, and tertiary folds. The lining epithelium is pseudostratified columnar rich in apical secretory granules. The lamina propria is wide and contains gland-like structures representing cut sections of the extremely folded mucosa.
- Musculosa: relatively thin and formed of inner circular and outer longitudinal smooth muscle fibers.
- Adventitia: thin fibroelastic connective tissue that binds the seminal vesicle to the surrounding structures.
Functions of the seminal vesicle
- The seminal vesicle is not a reservoir for spermatozoa It secretes a mucoid yellowish seminal fluid, forming a large part of the human ejaculate (semen), into the ejaculatory duct shortly after the vas deferens empties the sperm.
- Seminal fluid contains fructose, a major source of energy for sperms motility as well as large quantities of prostaglandins and fibrinogen.
- Prostaglandins are believed to aid fertilization in two ways:
- Reacting with the thick cervical mucus to make it more receptive to sperms movement.
- Causing reverse peristaltic contractions in the uterus and Fallopian tubes to move the sperms toward the ovum (a few sperms reach the upper ends of the Fallopian tubes within 5 minutes).
Ejaculatory duct
It is about 2 cm long. It is formed by the union of the duct of the seminal vesicle and the terminal part of the vas deferens, close to the base of the prostate. The ejaculatory duct penetrates the base of the prostate, and passes anteroinferiorly to open into the prostatic urethra.
It is lined by columnar epithelium and then by transitional epithelium as it opens into the prostatic urethra. The ejaculatory duct does not have musculosa in its wall. Ejaculatory ducts mix sperms with seminal fluid and then deliver semen to the urethra where prostatic secretion is added.
You can download Science online application on Google Play from this link: Science online Apps on Google play
Organs of male genital system, Structure of the testis, Functions of Sertoli cells & Leydig cells
Testis functions, sperms production, Factors affecting spermatogenesis, Structure of Epididymis
Prostate function, structure, lobes, Benign enlargement of prostate & malignant prostatic tumor
Testosterone effects, low testosterone symptoms, Hypogonadism & Hypergonadism in male