Posterior pituitary gland hormones and function, Control of ADH and Oxytocin hormone
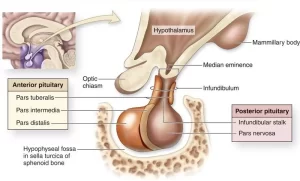
The pituitary gland is known as the hypophysis, It is an endocrine gland about the size of a pea. It is divided into two parts which are the anterior pituitary & the posterior pituitary, The posterior pituitary or neurohypophysis is the posterior lobe of the pituitary gland which is part of the endocrine system, It is not glandular as is the anterior pituitary, It stores and secretes two hormones made in the hypothalamus, and it does not produce any hormones of its own.
Hormones of Posterior Pituitary
- Antidiuretic Hormone (ADH).
- Oxytocin Hormone.
Antidiuretic Hormone and Oxytocin Hormone are synthesized in the hypothalamus and stored in the posterior pituitary gland.
Functions of Antidiuretic Hormone (Vasopressin, ADH):
A) On the kidneys:
ADH increases the reabsorption of water by the kidney, These reduce the excretion of water from the body, The urine becomes concentrated and its volume is reduced (antidiuretic effect), It acts on the distal portions of nephrons (in the collecting duct and collecting tubules), increasing their permeability to water, ADH causes the opening of many protein water channels.
B) On the Blood vessels
ADH is a potent vasoconstrictor, it acts on vascular smooth muscle, ADH in moderate concentration has a very potent effect of constricting the arterioles so, increasing the arterial pressure. Under normal conditions, this action does not significantly alter arterial pressure because it is counteracted by the baroreceptor reflexes. The vasoconstrictor of ADH is important in the maintenance of arterial pressure in hypotensive conditions, such as hemorrhage.
The effect of ADH on the kidney has more physiologic importance. Under normal conditions, vasopressin is the primary endocrine factor that regulates urinary H2O loss and overall H2O balance. In contrast, typical levels of vasopressin play only a minor role in regulating blood pressure by means of the hormone’s pressor effect.
Control of ADH
1- Osmotic stimuli
The release of ADH is controlled by a feedback mechanism that acts to maintain the plasma osmolality close to 290 mOsm/L. When the osmolality of the plasma is increased (as in dehydration or high salt level) the rate of discharge of vasopressin from the posterior pituitary increases leading to water retention by its action on the kidney.
The change in osmolality is sensed by osmoreceptor cells present in the hypothalamus which transmit signals to cell secreting ADH (supraoptic and paraventricular nuclei). Plasma osmolality changes of as little as 1-2% are detected by hypothalamic osmoreceptors.
2- Volume depletion
A decrease in circulatory volume and mean arterial pressure will increase ADH. They are sensed by low-pressure receptors in the vascular system which are the primary mediates of volume effect on ADH secretion (in the atria, pulmonary vessels, great veins).In hemorrhage, ADH is secreted in large amounts. It promotes water conservation to reestablish the circulatory volume and causes vasoconstriction to maintain blood pressure.
Decreased extracellular fluid volume (without change in osmolality) stimulates thirst and ADH secretion (e.g. hemorrhage): However, small decreases in volume have minimal effect on ADH levels.
Antidiuretic hormone deficiency (Diabetes Insipidus)
- Polyuria: Excretion of a large amount of dilute urine. The urine-specific gravity remains almost constantly between 1002-1006. The urine output is usually 4 to 6 liters per day and up to 18 liters.
- Polydipsia: The rapid loss of fluid in urine creates a constant thirst. If the sense of thirst is depressed for any reason and the intake of dilute fluid decreases, the patient develops dehydration and hypernatremia with hyperosmolarity that can be fatal.
Oxytocin
Functions of Oxytocin hormone:
A- in Female:
- Milk ejection causes the contraction of special smooth muscle-like cells known as myoepithelial cells that line the alveoli and ducts of the mammary gland thus squeezing milk outwards through the nipple.
- Contraction of the smooth muscle of the uterus: It causes contraction of the smooth muscle fibers of both pregnant and non-pregnant uterus. It is used clinically for the induction of labour. It plays a role in initiating labour and its secretion is increased during labour. It acts on the non-pregnant uterus to facilitate sperm transport by contraction of the uterus.
- In addition to these two major physiologic effects, oxytocin has been shown to influence a variety of behaviors, especially maternal behaviors, For example, this hormone facilitates bonding, or attachment, between a mother and her infant.
B- In male:
The functions of oxytocin are not definitely known. It has been suggested that it causes a discharge of sperms from the seminiferous tubules and epididymis to the vas deferens.
Control of Oxytocin Secretion
- Suckling reflex: The suckling of the breast stimulates touch receptors in the nipple, and sensory nerves transmit impulses upward to the hypothalamus to cause the release of oxytocin. The oxytocin is then carried by the blood to the breasts where it causes contraction of myoepithelial cells that lie outside and surrounding the alveoli of the mammary gland, in less than a minute after the beginning of suckling, milk begins to flow this is called milk-ejection.
- Stretching of the uterine cervix, as occurs during labour can cause a neurogenic reflex that causes the posterior pituitary to increase its secretion of oxytocin to enhance labor.
- Genital stimulation: The secretion of oxytocin is increased by genital stimulation.
You can follow Science Online on YouTube from this link: Science online
Regulation of Growth Hormone Secretion and Effects of Deficiency of Anterior Pituitary Hormones
Anterior pituitary gland function, hormones, location and Effects of Growth Hormone
Pituitary gland function, structure, location, hormones and anatomy
Endocrine system structure, function, disorders, Endocrine Glands and Hormones types
Endocrine system, Endocrine glands, Pituitary gland and Hormonal coordination in living organisms
Thyroid gland function, hormones, function, anatomy and Congenital anomalies