Anomalies of renal pelvis and ureter, Pelvi-Ureteric Junction Obstruction and Ureterocele
Anomalies of the renal pelvis and ureter are structural variations from the normal anatomy of these parts of the urinary system. These anomalies can be present at birth (congenital) or acquired later in life. Some anomalies may not cause any problems, while others can lead to complications such as urinary tract infections, kidney stones, or kidney damage.
Anomalies of the renal pelvis and ureter
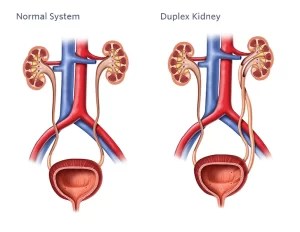
Duplication: This is the most common anomaly, where there is a double collecting system for one or both kidneys. This can cause problems if one ureter is blocked or if the two ureters do not drain urine properly.
Ectopic ureter: This occurs when the ureter inserts into an abnormal location, such as the urethra, vagina, or seminal vesicle. This can cause incontinence or recurrent urinary tract infections.
Ureteropelvic junction (UPJ) obstruction: This is a blockage at the junction where the ureter connects to the renal pelvis. This can cause urine to back up into the kidney and lead to kidney damage.
Pelvic diverticulum: This is a pouch that forms in the wall of the renal pelvis. It can trap urine and increase the risk of infection.
Megaureter: This is an enlarged ureter. It can be caused by a blockage or by a weakness in the ureter wall.
If you are experiencing any symptoms that may suggest a renal pelvic or ureteral anomaly, such as pain in the flank, blood in the urine, or frequent urination, it is important to see a doctor for diagnosis and treatment.
1. Pelvi-Ureteric Junction Obstruction
Definition: a narrow ureteral segment (5-10 mm in length) at the pelvi ureteric junction.
Etiology:
- Atresia or achalasia in the ureteral wall.
- Compression of the pelvi-ureteric junction by an aberrant renal artery (an abnormal branch of the renal artery) hinders urine drainage into the ureter.
Diagnosis:
- Presented as prenatal hydronephrosis during antenatal care.
- Ultrasound will show increased anteroposterior diameter of the renal pelvis.
- MRU will show hydrocalices and hydropelvis with a normal caliber ureter below the pelvis.
- DTPA isotope scans to assess differential renal function and diagnose obstruction.
Treatment
Indications:
- Differential renal function is less than 40%.
- Anteroposterior diameter of the renal pelvis more than 4 cm.
Pyeloplasty: Surgical excision of the pelvi-ureteric junction and reconstructive anastomosis between the renal pelvis and the ureter, If there is an aberrant renal artery: The ureter is excised and re-anastomosed in front of the aberrant artery. The artery must always be preserved because it is always an end artery: it is the only source of blood supply to the lower pole of the kidney.
2. Duplication of the Renal Pelvis and Ureter
- Duplication can be confined to the renal pelvis (duplex pelvis) or also involves the ureter (incomplete or complete duplication).
- Incomplete duplication: 2 ureters arising from a duplex renal pelvis. They join at any level to form one stem that opens as a normal ureter in the bladder.
3. Ureterocele
Etiology
Congenital stenosis of a ureteric orifice ⇒ high intra-ureteral pressure ⇒ distension and ballooning of the ureteral wall into the bladder cavity ⇒ ureterocele. The weak anterior and lateral ureteral walls caused by the absence of ureteral muscle at the level of the ureteric orifice facilitate the herniation (review “Anatomical Consideration” under Renal Agenesis).
Pathology
- A ureterocele appears as a balloon that bulges in the bladder cavity with a ureteric orifice at its tip.
- Ureterocele is usually small and unilateral but can be huge and bilateral.
- The wall of the ureterocele is devoid of muscle. It is lined by 2 layers of urothelium: ureteral mucosa from the inside, and bladder mucosa from the outside.
Diagnosis
I. Intravenous urography:
- If the kidney is functioning, contrast will fill both the ureterocele cavity and the bladder cavity. Both cavities are separated by a linear filling defect that represents the wall of the ureterocele (cobra head appearance).
- If the kidney is non-functioning, the ureterocele cavity will not contain contrast. Contrast reaching the bladder from the opposite kidney will fill the bladder cavity. The ureterocele will thus appear as a filling defect (shifted to one side and has a regular outline).
II. Cystoscopy: The ureterocele is seen as a balloon bulging into the bladder cavity. It is lined by bladder mucosa with the ureteric orifice at its tip.
Complications
- Hydroureter and hydronephrosis secondary to a narrow ureteric orifice.
- Urinary tract infection and stone formation in a big ureterocele with stagnant urine.
Treatment
- Endoscopic treatment: Transurethral incision of the ureterocele wall using a special knife connected to electrical current through the resectoscope, for drainage of the ureterocele in the presence of infection.
- Surgical treatment:
- Functioning kidney unit: Excision of the ureterocele followed by re-implantation of the ureter to the bladder by an anti-reflux procedure.
- Nonfunctioning kidney unit: excision of the ureterocele, ureter, and the kidney unit.
3. Vesico-Ureteral Reflux
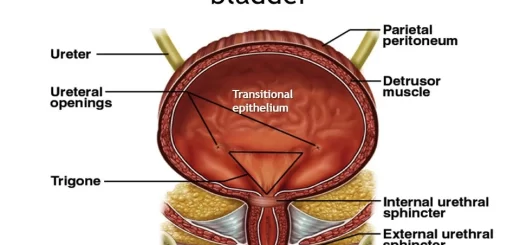
Anatomical Consideration: The intravesical (terminal part) ureter runs an oblique course inside the bladder wall downwards and medially ends in the ureteric orifice. The oblique course of the intravesical ureter prevents reflux from happening, as during voiding the intramural and the submucosal portions of the ureter are compressed against the packing of the detrusor muscles of the contracting bladder (flap valve mechanism) preventing the reflux of urine back into the ureters.
Types
1. Primary VUR
In the absence of outflow obstruction or anatomical abnormalities. The intravesical ureter is congenitally short and lateral in position not reaching its normal position in the trigone. It runs vertically (not obliquely) across the bladder wall to open in a wide patulous ureteric orifice. This abnormal course results in the absence of the flap valve mechanism and will lead to vesico- ureteral reflux. The condition is either unilateral or bilateral.
2. Secondary VUR
Associated with abnormal bladder function and elevated intravesical pressure e.g. neurogenic bladder and posterior urethral valve.
Diagnosis
- Voiding cysto-urethrogram (VCUG): contrast passes from the bladder up to the ureter.
- Cystoscopy: a patulous ureteric orifice is seen suggestive of reflux.
Grading
- Grade 1: Reflux filling of the distal ureter (lower third).
- Grade 2: Reflux filling of the whole ureter (lower and upper third).
- Grade 3: Reflux filling of the renal pelvis.
- Grade 4: Reflux filling of the renal pelvis and calyces.
- Grade 5: Reflux filling of the renal pelvis and calyces, with tortuosity of the ureter.
Complications
- Recurrent UTI causes reflux pyelonephritis that will lead to scarring of the renal parenchyma and may end by loss of renal function.
- Hydroureter and hydronephrosis caused by functional (not organic) obstruction: urine passing down from the ureter to the bladder is faced with resistance by urine refluxing from the bladder up the ureter.
Treatment
1. Grade 1-3: Usually self-limited (it can regress spontaneously with puberty). It requires no treatment, unless it persists and causes complications.
2. Grade 4 and 5 complications are treated surgically by mobilization of the ureter inside the bladder in the submucosa to increase the intravesical length and produce an anti-reflux mechanism.
You can subscribe to Science Online on YouTube from this link: Science Online
You can download Science Online application on Google Play from this link: Science Online Apps on Google Play
What are genitourinary disorders?, Kidney anomalies, Renal Cysts and Malrotated Kidney
Functions of Kidneys, Role of Kidney in glucose homeostasis, Lipid & protein metabolism
Urinary system structure, function, anatomy, organs, Blood supply & Importance of renal fascia
Suprarenal glands (adrenal glands) anatomy, structure & Effect of Deficiency of Catecholamines
Histological structure of kidneys, Uriniferous tubules & Types of nephrons
Urine formation, Factors affecting Glomerular filtration rate, Tubular reabsorption & secretion
Functions of the loop of Henle, distal tubules, collecting ducts & Glucose tubular maximum