Functions of the loop of Henle, distal tubules, collecting ducts and Glucose tubular maximum
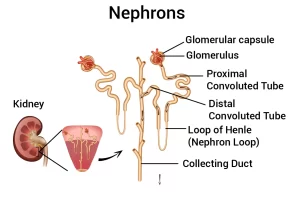
Loop of Henle (or Henle’s loop, Henle loop, nephron loop) is the portion of a nephron that leads from the proximal convoluted tubule to the distal convoluted tubule in the kidney. It creates a concentration gradient in the medulla of the kidney, It creates an area of high urea concentration deep in the medulla, near the papillary duct in the collecting duct system.
Reabsorption in the loop of Henle
The Henle loop functions include Homeostatic mechanisms to regulate the extracellular fluid volume, Regulating potassium, calcium, and magnesium excretion at the lowest energy costs, Homeostasis of the acid-base balance via bicarbonate, and ammonia excretion, Regulating the composition of urinary protein.
The thin descending limb
It has relatively low permeability to solutes and lacks mechanisms for active solute transport but is highly permeable to water. Water is reabsorbed from the tubular fluid and its osmolality increases as it flows through the thin descending limb.
The ascending limb
The ascending limb of juxtamedullary nephrons can be divided into two regions: the thin ascending limb which begins at the hairpin turn, and the thick ascending limb, which begins at or near the junction between the inner and outer medulla, In contrast, cortical nephrons lack a thin ascending limb, the thick ascending limb, therefore begins near the hair-pin turn.
The thin ascending limb of juxtamedullary nephrons
The thin ascending limb is impermeable to water but highly permeable to sodium and chloride ions, Sodium and chloride ions diffuse passively from the lumen to the medullary interstitial space.
The thick ascending limb
The water permeability of the thick ascending limb is negligible, It actively transports sodium ions, while chloride and potassium ions transport is secondary active to sodium (sodium Co-transport), therefore, the osmolality and the concentration of sodium and chloride of the tubular fluid decrease, The tubular fluid that leaves the loop of Henle is hypotonic.
Summary of functions of the loop of Henle
- The Henle loop has an important role in the mechanisms for both urinary concentration and urinary dilution.
- Reabsorption of 15-20% of the filtered water.
- Reabsorption of 25% of the filtered sodium and potassium.
- Reabsorption of chlorides.
Functions of distal tubules & collecting ducts
- Active reabsorption of 8-10% of the filtered sodium.
- Active secretion of potassium and hydrogen ions under the control of the aldosterone hormone.
- Reabsorption of up to 15% of the filtered water “Facultative water reabsorption” which is under the control of ADH.
- Reabsorption of urea from the inner medullary part of the collecting duct which is facilitated by ADH. The rest of the tubular epithelium is impermeable to urea.
In this part of the nephron, the volume of urine and its content of sodium, potassium, and hydrogen ions are adjusted according to the water, electrolyte, and acid-base balance of the body.
Tubular transport maxima
The tubular maximum is a term given to indicate the maximum amount of a substance in mg, which can be absorbed or secreted per minute. Under normal conditions, it remains constant for the individual, The glucose tubular maximum (TmG) measures the absorbing power of the tubules, The tubular maximum for Para-Amino-Hippuric acid (TMPAH) measures the secretory power of the tubules.
Glucose tubular maximum (TmG)
Glucose absorption needs a carrier. The amount of this carrier is limited and so the amount of glucose absorption is limited. The maximum capacity of tubular cells to reabsorb glucose is called tubular maximum for glucose or TmG.
The glucose tubular maximum is determined by increasing the glucose concentration in the plasma insteps and determining the amount of glucose excreted in the urine, The difference between the quantities of glucose filtered and those excreted represents the amount absorbed by the tubules, The amount of glucose filtered per minute is calculated (concentration of glucose per ml plasma X GFR). The amount of glucose excreted in urine is calculated (concentration of glucose per ml urine X volume of urine per minute).
Within the physiological range of blood glucose level (80-180 mg/100ml), all glucose filtered is reabsorbed by the tubules and none is excreted in the urine. At the critical or threshold level (about 180 mg%) glucose starts to be excreted in urine (Glucosuria) because the absorbing power of some tubules becomes saturated.
With a gradual increase of blood glucose concentration above the threshold value, more renal tubules become saturated until all the tubules become saturated. At a higher concentration, no increase in glucose absorption occurs. The excess of glucose filtered is excreted in urine because the tubules reach their maximum absorbing capacity which is about 375 mg/min. for men and 300 mg/min. for women.
Para-Amino-Hippuric acid tubular maximum (Tm PAH)
PAH tubular maximum measures the secretory power of the tubules. If PAH is administered intravenously in a small amount so as to maintain a low concentration in blood, it is found that the blood leaving the kidney in the renal vein contains 10% of PAH, 90% of PAHs removed from the renal blood in a single circulation, by filtration, and by secretion.
If PAH concentration in plasma is increased, the rate of tubular secretion increases until a maximum is reached and no further augmentation of secretion occurs. This denotes that the tubules have a limit for the secretory power. Tm PAH equals 75 mg/min.
You can subscribe to science online on YouTube from this link: Science Online
You can download Science Online application on Google Play from this link: Science Online Apps on Google Play
Transport through Renal tubules, Kidney Transport & function of proximal convoluted tubules
Urine formation, Factors affecting Glomerular filtration rate, Tubular reabsorption & secretion
Histological structure of kidneys, Uriniferous tubules & Types of nephrons
Functions of Kidneys, Role of Kidney in glucose homeostasis, Lipid & protein metabolism
Urinary system structure, function, anatomy, organs, Blood supply & Importance of renal fascia
Osmolality, Concentrating mechanism of the kidney, Urine concentration & dilution