Control of water balance in your body, Regulation of volume and osmolality of Body fluids
The principal function of the kidneys is to control almost all the characteristics of body fluids, especially the ECF. Such characteristics are: volume, composition, and osmolality. Maintenance of normal volume and osmolality of body fluids requires that the input of solvent and solutes to the body equals their output from the body each day. This principle, input = output, is referred to as balance.
Regulation of volume & osmolality of the body fluids
Since the major extracellular solute is Na+ (along with its linked anions), the regulation of the volume and osmolality of the ECF is dependent almost exclusively upon the regulation of the balances of water and Na+.
Water balance
Input of water
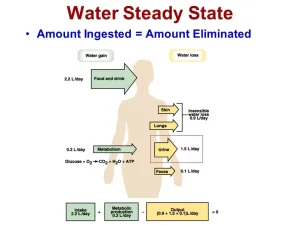
Water is added to the body fluids from 3 sources:
- The water content of food: About 800-1000 ml/day.
- Water generated during the oxidation of food: About 300-400 ml/day.
- Water consumed as a liquid: 1-2 liters/day.
The total water input = 2100-3400 ml/day
Output of water
Water is lost from the body through 4 routes:
- Insensible loss: Averages about 800-1000 ml/day, half of which is lost as moisture in expired air, and half is lost as water that evaporates through the skin (water of perspiration).
- Sweat can vary from less than 200 ml/day in an individual at rest in a cool environment to as much as 8-10 L/day if the environmental temperature, humidity, and/or level of physical activity are increased.
- Fecal loss: In a normal man is only 100-200 ml/day.
- Urine: Averages 1-2 liters/day.
The total water output = 2100-3400 ml/day.
The body is unable to prevent insensible water loss, sweat, or fecal loss. Therefore, these outputs of water are called obligatory losses. In addition, part of urine output can be regarded as obligatory which is about 500-600 ml of the daily urine volume.
Control of water balance
The input and output of water are regulated by changes in the volume of liquid ingested and urine volume, which in turn are controlled by the plasma level of ADH and thirst. Moreover, water balance is affected indirectly by mechanisms that regulate sodium balance.
1. Secretion of ADH
Two neuronal areas are important in controlling osmolality and ADH secretion.
a) The hypothalamus
The hypothalamus contains 2 areas that are important in controlling ADH secretion:
- The supraoptic nuclei: about five-sixths (5/6) of ADH are formed in the cell bodies of their neuronal cells.
- The paraventricular nuclei: the remaining one-sixth (1/6) of ADH is formed here.
b) AV3V region
A second broad neuronal area is located along the anteroventral region of the third ventricle (AV3V) contains neuronal cells that are excited by very minute increases in ECF osmolality. These neurons are called osmoreceptors (osmosodium receptors). They send signals to the supraoptic nuclei to control the secretion of ADH. It is likely that they also induce thirst as well.
2. Thirst sensation
The thirst center is located in:
- The AV3V region.
- Small areas in the preoptic hypothalamus.
Mechanisms regulating water balance (ADH-thirst system)
A. Increase in plasma osmolality
The increase in plasma osmolality is produced by:
a) Excess sodium and the negative ions that go with it excite the osmoreceptors located in the hypothalamus which causes the release of ADH that increases the permeability of the late distal tubules and collecting ducts, causing increased conversation of water by the kidneys.
The conservation of water with the loss of sodium and other osmolar substances in the urine causes dilution of the sodium and other substances in the ECF, thus correcting the initial increase in plasma osmolality.
b) Decrease in blood volume (total body water).
Mechanism exciting the osmoreceptors (orosmosodium receptors)
Increased osmolality in the ECF pulls water out of the osmoreceptors, causing them to shrink and thereby increasing their rate of discharge. The osmoreceptors respond to changes in ECF sodium concentration but not to changes in potassium concentration and only slightly to changes in urea and glucose concentrations. The reason is probably that these substances can penetrate the osmoreceptors cell membranes and therefore cause little or no osmotic effect.
B. Decrease in blood volume
The decrease in blood volume causes the arterial pressure to fall and activates the arterial baroreceptor reflex. Moreover, the volume receptor reflex is activated when the pressures in the two atria, in the pulmonary artery, and in other low-pressure areas of the lesser circulation fall below normal. The net result is to activate the ADH-thirst system and thereby increase the body fluid volume.
You can subscribe to science online on YouTube from this link: Science Online
You can download Science Online application on Google Play from this link: Science Online Apps on Google Play
Osmolality, Concentrating mechanism of the kidney, Urine concentration & dilution
Urine formation, Factors affecting Glomerular filtration rate, Tubular reabsorption & secretion
Histological structure of kidneys, Uriniferous tubules & Types of nephrons
Functions of Kidneys, Role of Kidney in glucose homeostasis, Lipid & protein metabolism
Urinary system structure, function, anatomy, organs, Blood supply & Importance of renal fascia