Anemias causes, symptoms, features, diagnosis and Types of Polycythemia
Anemia means a deficiency of red blood cells and/or decreased hemoglobin concentration 2 grams below the normal mean for a person, i.e. below 14 g/dl for men and below 12 g/dl for women. Microcytic hypochromic anemias are most often due to iron deficiency in the diet or chronic blood loss with loss of large amounts of iron over a long period.
Causes of anaemia
- Loss of red blood cells e.g. bloodless anemia.
- Destruction of red blood cells e.g. haemolytic anemia.
- Decreased or defective production of red blood cells by the bone marrow e.g. aplastic anemia and nutritional anemias.
Blood loss anemia
- Acute loss of red cells as in sudden haemorrhage (car accidents, surgery).
- Chronic loss of red blood cells as in bleeding gums, peptic ulcer, bleeding piles, and excessive uterine bleeding.
Haemolytic anemia
This can result from several factors: Infections such as malaria, Reactions to certain drugs, e.g. sulphonamides, Autoimmune disorders. The body forms antibodies against its own red blood cells, Hemolytic disease of the newborn: Erythroblastosis fetalis, where the Rh-positive red cells in the fetus are destroyed by antibodies from an Rh-negative mother. Hereditary abnormalities of red blood cells such as sickle cell anemia and favism.
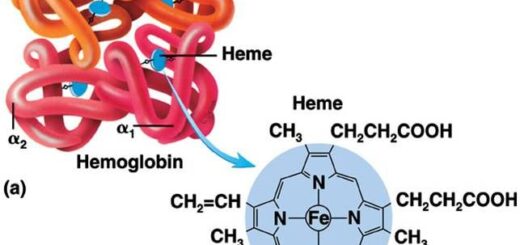
In sickle cell anemia, the cells contain an abnormal type of hemoglobin called hemoglobin-S. When this hemoglobin is exposed to low O2 concentration, it precipitates into long crystals inside the red cells. These crystals elongate and cause the red cells to become sickle-shaped, hemolyze, and form aggregates that block blood vessels. In Favism, Deficiency of glucose-6-phosphate dehydrogenase enzyme. Acute hemolysis is induced by eating fava beans.
Aplastic and nutritional anemias
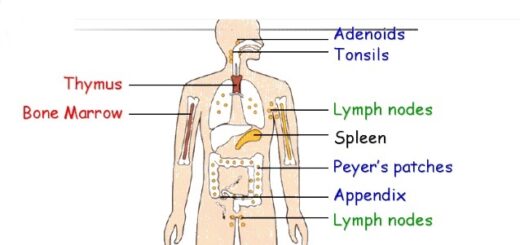
- Aplastic anemia: Bone marrow aplasia means a lack of functioning bone marrow. This could result from excessive X-ray or gamma-ray irradiation, industrial chemicals, or drugs.
- Nutritional anemias: Deficiency of iron, proteins, vitamin B12, or folic acid can lead to very slow production of the erythroblasts in the bone marrow and thus, anemia may develop.
Morphologic classification of anemias
According to red cell volume (mean corpuscular volume, MCV) and mean cell hemoglobin (MCH), anemia is classified into:
Normocytic normochromic anemias occur in acute haemolytic anemia and in acute blood loss. Characteristics: Decreased red cell count, Decreased blood hemoglobin concentration, Decreased hematocrit, The red cells are of normal size (normocytic) and of normal hemoglobin content (normochromic).
Microcytic hypochromic anemias are most often due to iron deficiency in the diet or chronic blood loss with loss of large amounts of iron over a long period. Characteristics: Red blood cells are small in size (microcytic), The hemoglobin content of each cell is less than normal (hypochromic), and the red cell count is slightly reduced.
Macrocytic normochromic anemias are associated with megaloblastic erythropoiesis due to the deficiency of vitamin B12 and folic acid. The deficiency of either vitamin B12 or folic acid causes maturation failure in the process of erythropoiesis. Vitamin B12 and folic acid are important for DNA synthesis.
Lack of these vitamins causes abnormal and diminished DNA and, consequently, the failure of nuclear maturation and cell division. Thus the erythroblastic cells of the bone marrow fail to proliferate rapidly, resulting in the production of macrocytes, which are irregular, large, and oval instead of the usual biconcave disc.
These poorly formed cells, after entering the circulation, are capable of carrying oxygen normally but are fragile with a short life. Characteristics: Red cells are large in size (macrocytic), The hemoglobin content of each cell is normal (normochromic), Reduced red cell count, and decreased hematocrit.
Pernicious anemia
Pernicious anemia is a macrocytic anemia that is combined with nervous system abnormalities. It results from vitamin B12 deficiency. Animal food is the main dietary source of vitamin B12. After ingestion, vitamin B12 normally combines with “the intrinsic factor” (a glycoprotein secreted by parietal cells of the stomach). It protects vitamin B12 from digestion by gastrointestinal enzymes and facilitates its absorption in the ileum.
Once the B12– intrinsic factor complex is absorbed, the intrinsic factor is released and the vitamin is transferred to the plasma. Vitamin B12 is stored in large quantities in the liver and is released slowly as needed by the bone marrow and other tissues. The normal liver can store enough vitamin B12 to meet the requirements for many months.
The main cause of pernicious anemia is, therefore, defective vitamin B12 absorption, secondary to intrinsic factor deficiency. This occurs in cases of gastric mucosal atrophy, with a deficiency of gastric secretions.
Characters of pernicious anemia
Megaloblastic red cells. Degenerative lesions of the spinal cord. These do not occur with isolated folic acid deficiency and may be linked to defects in other reactions that depend on vitamin B12 as a cofactor.
Polycythemia
Polycythemia is an increase of red blood cells count and /or an increase of blood hemoglobin level 2 grams above the normal value.
Types of Polycythemia
Primary polycythemia (polycythemia Vera) is a tumorous condition of the bone marrow that causes excess production of red blood cells. Secondary polycythemia (physiological) occurs secondary to hypoxia leading to an increase in the production of red blood cells:
- High altitude: the tissues become hypoxic due to decreased O2 tension in the atmosphere leading to increased production of erythropoietin which stimulates red cell formation by the bone marrow.
- Polycythemia of the fetus: the fetal hemoglobin has a great affinity to O2 and it gives the tissues less O2 than adult hemoglobin leading to hypoxia, increased production of erythropoietin and polycythemia.
- Pulmonary and heart diseases: failure of delivery of O2 to the tissues leads to increased production of red blood cells.
Effects of polycythemia
An increase in red blood cell count increases the oxygen-carrying capacity of the blood. The increased red blood cell volume is detected by an increased haematocrit value. In severe polycythemia, the hematocrit value may reach 70% instead of the normal 45%. This would greatly raise the blood viscosity, increase the arterial blood pressure, and the work done by the heart. It is also associated with sluggish peripheral circulation.
Case study
A 50-year-old man comes to his physician complaining of fatigue. He says that climbing the stairs leaves him short of breath and this has been getting progressively worse over the past month. The patient works in a stressful job and to relieve the stress he smokes and drinks 6 cups of coffee a day. He has been taking aspirin for the last 6 months for frequent knee pain.
His tests revealed: Hematocrit: 30%, Red blood cell smear: Microcytic hypochromic cells, Serum iron: 27 μg/dL, Transferrin saturation: 13 %, and stool test: positive for occult blood.
Diagnosis and treatment
The patient is diagnosed with iron-deficiency anemia caused by chronic blood loss from a stomach ulcer that was exacerbated by repeated aspirin intake. The bleeding is confirmed by the presence of occult blood in stools. The ulcer is treated medically and the patient is prescribed iron tablets with vitamin C to aid iron absorption.
Functions and sources of Folic acid, Cobalamin (vitamin B12) & Vitamin K
Factors that help iron absorption, Daily iron requirements & Abnormal iron levels
Red blood cells (Erythrocytes) structure & function, Myeloid tissue & Bone marrow
Hemoglobin structure, review & Types of normal hemoglobin
Abnormal types of hemoglobin, Sickling of RBCs, Types & causes of methemoglobinemia
Blood groups, Rh blood groups, Erythroblastosis fetalis & Importance of Rh factor