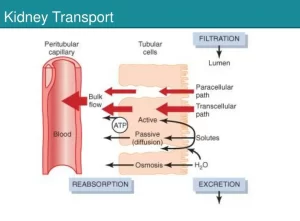
Transport through Renal tubules, Kidney Transport and function of proximal convoluted tubules
The basic mechanisms for transport through the tubular membrane are essentially the same as those for transport through other membranes of the body. These can be divided into passive transport or diffusion and active transport.
Active Transport
Active transport depends on the transport of substances by carrier proteins in the cell membrane. The carrier protein imparts energy to the substance to move it against an electrochemical gradient. The energy is derived from ATP. The active transport carrier proteins have an ATPase activity, which means that they can cleave ATP to form ADP or AMP with the release of energy from the high-energy phosphate bonds.
Active transport of sodium in the proximal convoluted tubules
On the basal and lateral surfaces of the tubular epithelial cell, the cell membrane contains extensive Na, K+ -ATPase that cleaves ATP, and the released energy transports sodium ions out of the cell into the interstitium and transports potassium ions from the interstitium to the interior of the cell.
The basolateral sides of the tubular epithelial cell are highly permeable to potassium that all the potassium diffuses back out of the cell into the interstitium. This sodium transport outward from the cell diminishes the sodium concentration and increases the negativity inside the epithelial cells to approximately 70 millivolts.
This causes the diffusion of sodium from the tubular lumen into the cell according to the “electrochemical” gradient. A carrier protein in the membrane enhances the movement of sodium through the membrane by a process called “facilitated diffusion“.
Secondary active transport (Na Co-transport)
Both glucose and amino acids are transported from the tubular lumen through the brush border by a process called “Sodium Co-transport”. The glucose or amino acid molecule binds with the same sodium carrier molecule in the brush border that transports sodium ions through this membrane. Then, as the sodium diffuses inward through the membrane it pulls the glucose or amino acid along with it.
Once inside the epithelial cell, the sodium and the glucose or amino acid split from the carrier. The glucose or amino acid then diffuses through the basal membrane of the cell and thence into the peritubular capillaries by a carrier down their concentration gradient “facilitated diffusion”.
Active secretion
Active secretion occurs in the same way as active absorption except that the membrane transports the secreted substance in the opposite direction, from the brush border not from the sides of the cells e.g. hydrogen ions, potassium, and urate ions.
Primary active secretion
In the late distal convoluted tubule & cortical collecting duct:
- Primary active secretion of potassium: Potassium secretion occurs in the principal cells which contain Na+, K+ ATPase in the basolateral border that pumps sodium out of the cell into the interstitium, potassium ions are transported in the opposite direction to the interior of the cell. The lumina border is very permeable to potassium.
- Primary active secretion of hydrogen ions: The intercalated cells or dark cells secrete hydrogen ions by primary active secretion by H+-AT Pase.
Secondary active secretion of hydrogen ions in the proximal convoluted tubule
Hydrogen ions are secreted by secondary active transport from the interstitium into the tubules. This occurs by a protein carrier that transports sodium ions in and hydrogen ions outside the tubule, this is called Na+H+ counter-transport.
Passive Transport
Passive transport, or diffusion, means free movement of a substance by a concentration gradient, chemical, electrical, or both, electrochemical gradient.
Passive absorption of water by osmosis
When the different solutes are transported out of the tubule their total concentration decreases inside the tubular lumen but increases on the outside in the renal interstitium, This creates a concentration difference that causes osmosis of water in the same direction that the solutes have been transported, The different portions of the tubules have different permeabilities to water.
Passive absorption by diffusion
When water is reabsorbed by osmosis, the urea in the tubular fluid remains behind. Therefore, the concentration of urea in the tubular fluid rises, which creates a concentration difference of urea between the tubular and interstitial fluids. This causes urea to diffuse from the tubular fluid into the interstitium.
However, the permeability of the membrane for urea in most parts of the tubules is far less than that for water, which means that far less urea is reabsorbed than water. A large proportion of the urea remains in the tubules and is lost in the urine -usually over 50% of all that enters the glomerular filtrate.
Diffusion by electrical differences across the tubular membrane
When active reabsorption of sodium takes place at the tubule, chloride ions are absorbed with it to keep electrical neutrality.
Passive secretion
Ammonia is synthesized inside the tubular cells and then diffuses into the tubular lumen by a concentration gradient.
Functions of proximal convoluted tubules
Sodium reabsorption
Sodium ions are the most important ions that determine the osmotic pressure and the volume of the extracellular fluid. About 65% of sodium in the glomerular filtrate is actively reabsorbed from the proximal tubules.
Chloride and bicarbonate reabsorption
Chloride and bicarbonate reabsorption is a passive process created by diffusion by an electrochemical gradient through the tubular membrane.
Water reabsorption
The wall of the proximal tubule is freely permeable to water. Absorption of the solutes results in the passive transport of water by osmosis. 65% of water in the glomerular filtrate is reabsorbed by the proximal tubule; this fraction of water is called “obligatory water reabsorption”, since it is osmotically obliged to the absorbed solutes. It is not under the control of the antidiuretic hormone.
The fluid leaving the proximal tubule has the control of antidiuretic hormone. The fluid leaving the proximal tubule has the same osmolality (isotonic) to plasma and glomerular filtrate. Solutes that are not reabsorbed become concentrated in the tubular fluid because of the absorption of water. Such substances undergo diffusion by a concentration gradient provided that the membrane is permeable to them; in this manner, urea is absorbed.
Glucose reabsorption
Potassium reabsorption
Phosphate reabsorption
Secretion in the proximal tubules
You can subscribe to science online on Youtube from this link: Science Online
You can download Science Online application on Google Play from this link: Science Online Apps on Google Play
Urine formation, Factors affecting Glomerular filtration rate, Tubular reabsorption & secretion
Histological structure of kidneys, Uriniferous tubules & Types of nephrons
Functions of Kidneys, Role of Kidney in glucose homeostasis, Lipid & protein metabolism
Urinary system structure, function, anatomy, organs, Blood supply & Importance of renal fascia