Thyroid gland function, hormones, function, anatomy and Congenital anomalies
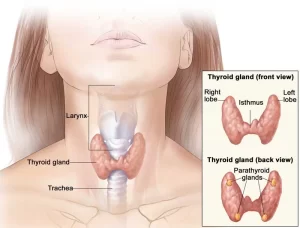
The thyroid is an endocrine gland, it is in the neck and it consists of two connected lobes, The lower two-thirds of the lobes are connected by a thin band of tissue called the thyroid isthmus. The thyroid gland makes two hormones and they are secreted into the blood: thyroxine (T4) and triiodothyronine (T3), These hormones are necessary for all the cells in your body to work normally.
Anatomy of thyroid gland
The thyroid gland is the largest endocrine gland in the body, its weight is 25 grams. Site: in the front & sides of the lower part of the neck clasping the trachea, extending from the level of the fifth cervical vertebra down to the first thoracic vertebra the ensheathed by the pretracheal fascia (layer by deep cervical fascia).
Shape: butterfly, consists of right and left lobes connected together as the median plane by a narrow part called the isthmus.
- 2 lateral lobes: each lobe is conical in shape with its superior pole diverging upwards and laterally to the level of the oblique lines of the thyroid cartilage. The lower poles diverge downwards and laterally reaching the level of the fifth tracheal ring.
- Isthmus: connecting the 2 lateral lobes.
- Small pyramidal lobe: (may be present) project upwards from the isthmus and may be connected by a fibromuscular band called levator glandulae thyroideae (remnants of thyroglossal duct in the embryo).
Extensions:
- The apex rests on the thyroid cartilage reaching its oblique line.
- Base: reach the level of 5, 6 tracheal rings
- The Isthmus: crosses opposite the 2, 3, 4 tracheal rings
Relations of the gland
I- The Isthmus
Anterior relations:
- Skin & superficial fascia.
- Anterior jugular veins.
- Deep fascia.
- Sternohyoid & sternothyroid.
Posterior relations:
Trachea (2, 3, 4 rings). The upper border of the isthmus is related to an anastomotic artery (between right & left superior thyroid arteries), The lower border of the isthmus gives rise of the right & left inferior thyroid veins, The pyramidal lobe may project upwards from the isthmus.
II- Thyroid lobes
Each lateral lobe has three surfaces: Anterolateral, medial, posterior surfaces
(1) Anterolateral surface (superficial surface):
- skin, superficial fascia (containing platysma muscle) & deep fascia pretracheal fascia.
- Its upper part is crossed by the superior belly of the omohyoid.
- Its middle part is covered by the sternohyoid (superficially) & sternothyroid (deeply).
- Its lower part is overlapped by the anterior border of the sternomastoid.
(2) Medial surface:
Its upper part is related to:
- Larynx thyroid, cricoid cartilages &cricothyroid muscle.
- Pharynx inferior constrictor muscle.
- External laryngeal nerve.
Its lower border is related to:
- a) Trachea.
- b) cervical Oesphagus.
- c) Recurrent laryngeal nerve (in between).
(3) Posterior surface:
Two parathyroid glands are embedded in the posterior surface of the gland
- inferior thyroid artery (before entering the gland).
- common carotid arteries (before inside the sheath).
- longus coli muscle.
The arterial supply to the thyroid gland
The thyroid gland receives its arterial supply from:
- The superior thyroid arteries (are the first anterior branch of the external carotid artery).
- Inferior thyroid arteries (arises from the thyrocervical trunk, a branch of the first part of the subclavian artery).
- Occasionally, the thyroideaima arteries (which arise from the arch of the aorta, brachiocephalic artery, or left common carotid artery. It supplies the isthmus of the thyroid gland).
Venous Drainage
Three pairs of veins provide venous drainage to the thyroid gland.
- The superior thyroid vein ascends along the superior thyroid artery at the apex of the lobe and it becomes a tributary of the internal jugular vein.
- The middle thyroid vein is a very short vein that arises from the middle of the lobe and ends in the internal jugular vein.
- The inferior thyroid veins: arises from the lower border of the isthmus and adjacent part of the lobes, They descend anterior to the trachea and collect into one vein which usually ends in the left innominate vein.
Applied Anatomy:
- Superior to the upper pole of the thyroid, the external laryngeal nerve runs with the superior thyroid artery before turning medially to supply the cricothyroid muscle, In 21% the nerve is intimately associated with the superior thyroid vessels, High ligation of the superior thyroid artery during thyroidectomy may cause injury of the external laryngeal nerve.
- The ligature of the inferior thyroid artery near the lower pole of the thyroid gland can lead to injury of the recurrent laryngeal nerve as they are near.
Development of thyroid gland
Origin: Thyroid bud develops from the floor of the pharynx opposite the first pouch between tuberculum impar and the copula of His.
Development:
- Bind end of the thyroid bud → dilates → descend caudally to the level of the Ultimobranchial body (4th pouch) which prevents its further descend in the thorax.
- The hollow distal bind end → solid flask-shaped → solid crescentic → sold bilobed.
- Endodermal cells of thyroid bud → thyroid follicles (thyroxine).
- Ultimobranchial body → parafollicular cells (C-cells) → calcitonin.
- The proximal part of the bud → narrow → stalk attached to the tongue thyroglossal duct → degenerate except at foramen caecum in the tongue.
Congenital anomalies of the thyroid gland
1- Persistent thyroglossal duct:
- The accessory thyroid tissue is formed from remnants of the duct.
- Thyroglossal cyst: lies inferior to hyoid bone at the midline of the neck (movable with deglutition & painless).
- Thyroglossal fistula: formed after rupturing of the cyst.
2- Ectopic thyroid gland:
- Lingual & sublingual thyroid due to incomplete descend → development inside or under the tongue.
- Retrosternal thyroid: due to excessive descend.
3- Agenesis due to failure of growth → critinism
4- Superficial thyroid lies superficial to the infrahyoid muscles.
In 50% part of the duct persists attached to the isthmus → pyramidal lobe.
You can follow Science Online on YouTube from this link: Science online
Regulation of Thyroid hormone secretion, Effects of Hyperthyroidism and Hypothyroidism
Regulation of Growth Hormone Secretion and Effects of Deficiency of Anterior Pituitary Hormones
Anterior pituitary gland function, hormones, location and Effects of Growth Hormone
Pituitary gland function, structure, location, hormones and anatomy
Endocrine system structure, function, disorders, Endocrine Glands and Hormones types
Endocrine system, Endocrine glands, Pituitary gland and Hormonal coordination in living organisms