Injuries to the Bladder and urethra, What are the complications of bladder injury?
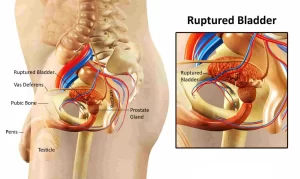
Injuries to the bladder, also known as bladder trauma, though not very common, can occur due to blunt or penetrating trauma to the lower abdomen. The bladder is a muscular sac that stores urine until you urinate.
Injuries to the Bladder
Symptoms of a bladder injury can include:
- Blood in the urine (hematuria).
- Pain in the lower abdomen or pelvis.
- Difficulty urinating (urinary retention).
- Inability to urinate (complete urinary retention).
- Bruising in the lower abdomen.
Treatment for a bladder injury
- Catheterization: A thin tube is inserted into the urethra to drain urine from the bladder, This may be necessary for a few days or weeks to allow the bladder to heal.
- Antibiotics: These medications may be prescribed to help prevent infection.
- Surgery: In some cases, surgery may be necessary to repair the bladder.
In most cases, a bladder injury heals completely with prompt medical attention. However, there can be complications from bladder injuries, such as Infection, Scarring, and Urinary incontinence (leakage of urine).
Cause of bladder injuries
- Blunt trauma. Road traffic accident or falling from height with fracture of the pelvic bones, bone fragments are the direct cause of injury.
- Penetrating trauma. Stab wound or gunshot especially with a full bladder.
- latrogenic. Perforation of the bladder during cystoscopy (for bladder tumor resection or stone crushing) or abdominoperineal surgery.
Types
1. Extraperitoneal rupture of the bladder.
a. Site: Areas not covered by peritoneum: lateral walls, posterior wall, and bladder base (all walls close to the bladder neck).
b. Presentation:
- Hematuria.
- Severe pelvic pain from the pelvic collection of a hematoma) (from bleeding fractured pelvic bones) + urinoma (extravasated urine)
c. Diagnosis:
i. Ascending cystogram (investigation of choice) will show:
- The contrast in the bladder escapes to the perivesical space or deeper in the pelvic cavity, depending on the extent of perforation.
- Compression and elongation of the bladder (inverted tear drop appearance) by a perivesical collection of urinoma and hematoma.
Contrast escapes to the pelvis. Bladder compression causes the “inverted tear drop appearance”
ii. CT cystography is also a valuable alternative to detect associated injuries
d. Management:
- A small perforation with minimal extravasation is managed conservatively by insertion of an indwelling wide-bore urethral Foley catheter for at least 1 week. This allows bladder healing while absorption of the urinoma occurs.
- A big perforation with excess urine extravasation is managed surgically by suturing the perforated bladder wall, insertion of cystostomy tube, draining the urinoma, and controlling pelvic bleeding.
2 Intraperitoneal rupture of the bladder:
a. Site: the bladder dome (covered by peritoneum).
b. Presentation:
- Hematuria and severe pelvic pain.
- Manifestations of the acute abdomen from intraperitoneal collection of urine that cause chemical peritonitis.
- The bladder is usually empty and the patient does not pass urine.
c. Diagnosis: Ascending (retrograde) cystogram: Contrast escapes from the bladder to the peritoneal cavity around the intestinal loops, CT cystogram is also more reliable.
d. Management: Immediate surgical drainage of urine from the peritoneal cavity, with suturing of the perforations (water-tight in a (double layer and placing a cystostomy tube and a drain in the peritoneum.
Urethral injuries
Anterior urethra: involves (penile and bulbar) urethra and it is covered by corpus spongiosum. Posterior urethra: involves membranous and prostatic urethra, it is not covered by corpus spongiosum and it is surrounded by the external and internal sphincter.
Etiology:
A. Anterior urethra: (usually iatrogenic causes).
- External trauma: fracture penis, bullet, falling astride.
- Internal trauma: during endoscopy or catheter insertion.
B. Posterior urethra:
- Mainly associated with pelvic fracture.
- Other causes include endoscopy, catheter insertion or during prostatectomy.
Presentation:
- History of the cause.
- Bleeding per-urethra (corner stone).
- Inability to void, with full bladder.
- Butterfly hematoma involving the perineum and scrotum.
- DRE may show a displaced prostate in association of a complete posterior urethral tear.
Investigations:
- A plain X-ray pelvis may show a pelvic bone fracture.
- An ascending urethrogram is a diagnostic tool that will show dye extravasation at the site of injury.
- Partial extravasation and the dye will reach the bladder.
- Complete extravasation and the dye will not reach the bladder.
Treatment:
If urethral injury is suspected Do not try to insert a catheter.
- Initial management: Suprapubic catheter insertion and primary realignment if possible.
- Delayed management: Urethroplasty after 3-6 months.
Complications:
- Urethral stricture. (narrow urethra lumen) treated by endoscopic visual urethrotomy or urethroplasty.
- Impotence.
- Incontinence.
Fracture penis
It is acute angulation of the penis during erection resulting into rupture of (tunica albugenia and hematoma formation secondary to escape of the blood outside the corpus cavernosum.
Symptoms and signs:
A popping or cracking sound, significant pain, swelling immediate loss of erection leading to flaccidity, and skin hematoma of various sizes are commonly associated with the sexual event (eggplant penis).
Investigations:
- Ultrasonography can detect the tunical tear and its site and extent.
- MRI is the best modality to diagnose tunical tear.
- Ascending urethrogram if urethral injury is expected (in cases of urethral bleeding). It is a rare condition.
Treatment:
- It is an emergency condition
- Evacuation of the hematoma.
- Suturing the edges of the tunica with vicryl 3/0 sutures.
Complications:
If left untreated, penile curvature secondary to fibrosis may occur or erectile dysfunction.
Torsion of the Testis
It is an emergency vascular insult of the testis, It results in the twisting of the spermatic cord with subsequent occlusion of the venous and arterial supply. If not treated within 4-6 hours after onset of pain the testis will undergo complete infarction and later atrophy.
Age:
- Bimodal
- Commonest in adolescence age 10-20 years.
- Less common in neonates.
Diagnosis:
Symptoms:
- Sudden severe testicular pain.
- Nausea and vomiting.
- High up testis.
Physical examination: tender testis, lie transversely,
Radiology: color Doppler US will show decreased blood flow in the testis.
Treatment:
It is an emergency and immediate surgical exploration is a must within 6 hours from the onset of torsion. Surgical exploration includes (detorsion) of the affected testis. If it is viable orchiopexy is done, if it is not viable orchiectomy is done. Contralateral orchiopexy should be done during the surgical exploration to protect the contralateral testis.
Differential diagnosis: Acute epididymitis and testicular trauma.
You can subscribe to Science Online on YouTube from this link: Science Online
You can download Science Online application on Google Play from this link: Science Online Apps on Google Play
Urolithiasis, Stones in the kidney or ureter, How do you treat urolithiasis?
Anomalies of the bladder and urethra, Urinary tract abnormalities symptoms
What are urinary tract infections?, kidney problems, Urinary retention and Bladder stones
Functions of Kidneys, Role of Kidney in glucose homeostasis, Lipid & protein metabolism
Histological structure of kidneys, Uriniferous tubules and Types of nephrons
Urine formation, Factors affecting Glomerular filtration rate, Tubular reabsorption and secretion
Urinary passages function, structure of Ureter, Urinary bladder & Uvulae vesicae
Urinary system structure, function, anatomy, organs, Blood supply and Importance of renal fascia
Urinary bladder structure, function, Control of micturition by Brain & Voluntary micturition