Antibacterial drugs definition, use and types, Penicillin classification and importance
Antibacterial drugs are derived from bacteria or molds or are synthesized de novo, “antibiotic” refers to antimicrobials derived from bacteria or molds but it is used synonymously with “antibacterial drug,” Antibiotics have many mechanisms of action, such as inhibiting cell wall synthesis, Increasing cell membrane permeability, Interfering with protein synthesis, nucleic acid metabolism, and other metabolic processes (eg, folic acid synthesis).
Antibacterial drugs
Many antibiotics are related and are grouped into classes, Although drugs within each class share structural and functional similarities, they have different pharmacology and spectra of activity. Antibiotics should be used only if clinical or laboratory evidence suggests a bacterial infection, Use for viral illness or undifferentiated fever is inappropriate in most cases.
Classification of antibacterial drugs
Classification of antibacterial drugs according to their mechanism of action:
- Cell Wall Synthesis Inhibitors: Beta-Lactams, Glycopeptides, and Bacitracin.
- Protein Synthesis Inhibitors: Aminoglycosides, Macrolides, Tetracyclines, Lincosamides, Chloramphenicol, and Linezolid.
- Nucleic Acid Synthesis Inhibitors: Fluoroquinolones, Metronidazole, and Rifampin.
- Bacterial Metabolism Inhibitors: Folate antagonists: Sulphonamides, Trimethoprim, and Pyrimethamine.
- Cell Membrane Inhibitors: Colistin.
- Specific Urinary Antiseptic Drugs: Fosfomycin, Nitrofurantoin.
Beta-lactam Antibiotics
Generally, if the pathogen is susceptible and the patient is non-allergic, beta-lactams, General features of Beta-lactams: are the preferred drugs for most situations due to their high efficacy, bactericidal nature, and good safety profile.
- None of beta-lactams has activity against Methicillin-resistant Staphylococcus aureus (MRSA), except Ceftaroline.
- None of them has activity against atypical intracellular organisms.
- They exhibit time-dependent killing: Their efficacy depends on the amount of time during which the drug concentration is above the MIC.
- They share features of chemistry, immunological characters, and mechanism of action.
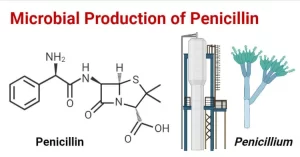
Penicillin
Penicillins are among the most widely effective and the least toxic drugs known, Members of this family differ from one another in the antimicrobial spectrum, stability to stomach acid, cross hypersensitivity, and susceptibility to bacterial degradative enzymes (B-lactamases).
Pharmacokinetics
Penicillin distributes well throughout the body, but they penetrate poorly into CSF and serous cavities, however infected serous membranes are more permeable, e.g. in meningitis, penicillin penetrates well.
All penicillin crosses the placental barrier, but none have been shown to have teratogenic effects. They are also excreted in breast milk and can be safely used during lactation.
The primary route of excretion is renal, therefore, patients with impaired renal function must have dosage regimens adjustment according to creatinine clearance, however, for nafcillin and oxacillin, as they are primarily metabolized in the liver, dose adjustment is not required in patients with renal insufficiency.
Classification
- Narrow spectrum beta-lactamase sensitive penicillin (natural Penicillin) include: Penicillin G, Acid resistant penicillin: penicillin V.
- Narrow-spectrum beta-lactamase-resistant penicillin (Anti-staphylococcal penicillin) includes nafcillin, oxacillin, cloxacillin, and dicloxacillin.
- Broad-spectrum penicillin includes ampicillin and amoxicillin.
- Extended-spectrum penicillin (Antipseudomonal penicillin) includes ticarcillin and piperacillin.
Narrow spectrum beta-lactamase sensitive penicillin (natural Penicillin)
They include penicillin G and penicillin V.
Spectrum
They are effective against Gram-positive cocci, Gram-positive bacilli, some Gram-negative cocci (Neisseria meningitides), non-beta lactamase-producing anaerobes, and Treponema palladium, Many bacterial species become resistant either by producing beta-lactamases (e.g. Staphylococcus aureus) or alteration of penicillin-binding protein (e.g., Streptococcus pneumonia).
Penicillin G includes:
- Crystalline penicillin G is given intravenously.
- Procaine penicillin is a long-acting preparation and is given intramuscularly once daily.
- Benzathine penicillin is a depot form, creating a stable low level of antibiotic for 2-4 weeks, Its therapeutic uses are:
- Prophylaxis against rheumatic fever: It is given as an intramuscular injection every 3-4 weeks against group A streptococcal reinfection.
- Treatment of primary, secondary, or early latent syphilis: A single intramuscular injection of long-acting benzathine penicillin.
- Group A streptococcal pharyngitis: As a single intramuscular dose.
Penicillin V is similar to penicillin G, but it is acid stable and is given orally, it is of limited use because of its poor bioavailability and frequent dosing 4-6 times per day.
Narrow spectrum beta-lactamase resistant penicillin
They include:
- Intravenous nafcillin and oxacillin.
- Oral cloxacillin and dicloxacillin.
These penicillins are resistant to staphylococcal beta-lactamases.
Spectrum
They are effective against staphylococci including those producing beta-lactamases, as well as streptococci.
Therapeutic uses
They are used for infections caused by Methicillin-sensitive Staphylococcus Aureus (MSSA).
Broad-spectrum penicillin (Amino-penicillin)
They include Ampicillin and amoxicillin. They are sensitive to beta-lactamases.
Pharmacokinetics
Amoxicillin is better absorbed from the gut, Its oral dose reaches approximately double the serum peak concentration of ampicillin and food does not interfere with its absorption, Because of more complete absorption of amoxicillin, the incidence of diarrhea is less than that of ampicillin.
Spectrum
In addition to activity against all organisms affected by standard penicillin, they have activity against non-beta lactamase-producing aerobic Gram-negative bacilli, e.g., influenzae, E.coli, and P.mirabilis, When used in higher doses or combined with beta-lactamase inhibitors, they gain broader spectrum.
Therapeutic uses
- Upper respiratory tract infection: Amoxicillin alone or in combination with a beta-lactamase inhibitor is recommended.
- Community-acquired pneumonia: High-dose amoxicillin alone or in combination with beta-lactamase inhibitor is recommended.
- Treatment of enterococcal endocarditis: Ampicillin with gentamicin.
- Meningitis: When risk factors for infection with L. monocytogenes are present e.g., in immunocompromised adults, empiric antibiotic treatment should include amoxicillin or ampicillin to cover that organism.
- Helicobacter Pylori eradication regimens in peptic ulcer diseases include amoxicillin.
Extended-spectrum penicillin (Anti-pseudomonal penicillin)
They include ticarcillin and Piperacillin.
Spectrum: They are sensitive to beta-lactamases. When combined with beta-lactamase inhibitors, their coverage includes Gram-negative organisms (including Pseudomonas aeruginosa), Gram-positive organisms, and anaerobic bacterial organisms.
Therapeutic uses
A combination of piperacillin-tazobactam is recommended for empiric therapy of hospital-acquired pneumonia, intra-abdominal infections, and septic shock.
Combined Penicillin/Beta-Lactamase Inhibitors
Beta-lactamases are a family of enzymes involved in bacterial resistance to beta-lactam antibiotics, They act by breaking the beta-lactam ring that allows penicillin-like antibiotics to work, Thus, combining beta-lactam antibiotics with a beta-lactamase inhibitor would protect them from destruction by beta-lactamases.
Beta-Lactamase Inhibitors
Clavulanate sulbactam and tazobactam are beta-lactamase inhibitors that have little intrinsic antibacterial activity but inhibit the activity of several beta-lactamases, For example:
- Amoxicillin/Clavulanate.
- Ampicillin/Sulbactam.
- Ticarcillin/Clavulanate.
- Piperacillin/Tazobactam.
Adverse Reactions
Penicillins are among the safest antibiotics, however, adverse reactions may occur in the form of:
1. Hypersensitivity reactions: Approximately 5% of patients have some reactions, ranging from rashes to angioedema and anaphylaxis. Cross-allergic reactions occur among the β-lactam antibiotics. There is no cross-allergenicity with monobactam.
2. Diarrhea: Diarrhea is a common problem that is caused by a disruption of the normal balance of intestinal microorganisms, Normal microflora is typically reestablished shortly after therapy is stopped, however, in some patients superinfection results, Pseudomembranous colitis, related to overgrowth and production of a toxin by Clostridium difficile, follows oral and, less commonly, parenteral administration of penicillin.
3. Neurotoxicity: Penicillins imitate neuronal tissue and they can provoke seizures if injected (intrathecally or if very high blood levels are reached, Epileptic patients are particularly at risk due to the ability of penicillin to Inhibit gamma amino butyric acid neurotransmission.
4. Hematologic toxicity: High doses of piperacillin, ticarcillin, nafcillin, and penicillin G has been associated with impaired hemostasis due to defective platelet aggregation, Cytopenia has been associated with therapy of greater than two weeks, and therefore, blood counts should be monitored weekly for such patients.
You can follow science online on YouTube from this link: Science online
You can download Science online application on Google Play from this link: Science online Apps on Google Play
Chemoprophylaxis indications, definition, examples & Causes of Misuse of antimicrobial drugs
Antimicrobial drugs types, use, side effects, resistance & Empiric antimicrobial therapy
Parasitic infections, Immunological tests, DNA probes and Polymerase Chain Reaction
Diagnosis of parasitic infections and Techniques used for identification of Intestinal Parasites
Myiasis classification, diagnosis, causes, treatment & medicolegal importance
Vaccines types, Live vaccines, Inactivated vaccines, Subunit vaccines, Naked DNA & mRNA vaccines