Chemoprophylaxis indications, definition, examples and Causes of Misuse of antimicrobial drugs
Chemoprevention is known as chemoprophylaxis, It refers to the administration of a medication for the purpose of preventing disease or infection, Antibiotics can be administered to patients with disorders of immune system function to prevent bacterial infections (particularly opportunistic infections), Antibiotics can be administered to healthy individuals to limit the spread of an epidemic, or to patients who have repeated infections (such as urinary tract infections) to prevent a recurrence.
Chemoprophylaxis
Chemoprophylaxis can prevent the spread of an existing infection in an individual to a new organ system, as when intrathecal chemotherapy is administered in patients with malignancy to prevent further infection. It can refer to the administration of heparin to prevent deep venous thrombosis in hospitalized patients.
Indications
- Presurgical antimicrobial prophylaxis: It is used to reduce the incidence of postoperative surgical wound infections. A single dose of cephalosporin (such as cefazolin) administered within one hour before the initial incision is appropriate for most surgical procedures.
- Antimicrobial prophylaxis in immunocompromised patients, eg. trimethoprim-sulfamethoxazole to prevent Pneumocystis pneumonia infection.
- Antimicrobial prophylaxis to prevent transmission of communicable pathogens to susceptible contacts, Ciprofloxacin can be given to close contacts of a patient with meningitis caused by N meningitides.
- Suppression of acquired infection before it causes an overt disease, e.g. chloroquine is given to the traveler to the malaria-endemic area for chemoprophylaxis.
- Prevention of mother-to-child viral transmission, e.g., antiretroviral drugs for HIV infection.
Antimicrobial selection
The choice of antibiotics depends on several factors either related to the drug itself or related to the patient.
Factors related to the drug
1. Drug’s pharmacokinetics/pharmacodynamics (PK/PD) profile
Dosing determinations for antimicrobials are based on achieving unbound drug concentrations that are above the minimum inhibitory concentration (MIC) of a pathogen, the level at which an antimicrobial inhibits the growth of the organism in vitro, Eventually, unbound drug levels decrease to less than the MIC, at which point any persistent antibacterial effect can be due to several causes.
- First, persistent suppression of microbial growth after brief exposure of microbe to an antimicrobial agent may occur, even in the absence of host defenses; this is the post-antibiotic effect (PAE).
- Second, after antibiotic exposure, organisms may be more susceptible than untreated pathogens to the antimicrobial activity of phagocytes, this is called post-antibiotic leukocyte enhancement.
- The dynamics of microbial killing by antimicrobial drug depends on either: the peak concentration (Cmax) relative to the MIC (concentration-dependent killing) or for how long the serum level stays above the MIC. This will affect the size of the doses and dosing intervals or duration of infusion time.
2 Access of antimicrobial drug to the site of infection
In addition to possessing in vitro antimicrobial activity and achieving adequate serum levels, the efficacy of antimicrobial agents depends on their capacity to achieve a concentration equal to or greater than the MIC at the site of infection.
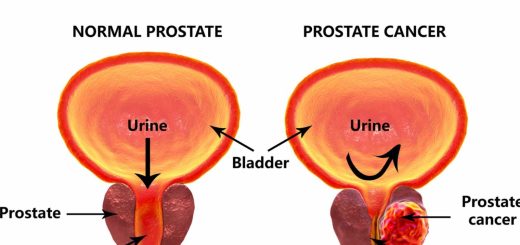
Antimicrobial concertions attained at some sites (e.g., ocular fluid, cerebrospinal fluid (CSF), abscess cavity, prostate, and bone) are often much lower than serum levels, For example, first-and second-generation cephalosporins and macrolides do not cross the blood-brain barrier and are not recommended for central nervous system infections, Fluoroquinolones achieve high concentrations in the prostate and are preferred oral agents for the treatment of prostatitis.
Agents in the same class can differ from one another, for example, moxifloxacin does not achieve significant urinary concentrations because of its low renal excretion and is therefore not suitable for the treatment of urinary tract infections (UTIs); in contrast, both levofloxacin and ciβprofloxacin are excellent choices for UTIs caused by susceptible bacteria.
Adverse effect profile
The adverse effects to antimicrobials may be direct or indirect. Direct adverse effects include allergy, toxicity, drug-drug interaction, and therapeutic failure, Indirect adverse effects include superinfection.
Allergy: The β-lactam drugs induce allergic reactions, Cross-reactivity occurs between drugs in similar chemical classes.
Serious toxicities:
- Nephrotoxicity (aminoglycosides).
- Hematologic toxicity (penicillins, linezolid, ganciclovir)
- QT interval prolongation (macrolides, fluoroquinolones, azoles).
- Hepatotoxicity (macrolides, azoles).
Superinfections: e.g., candida infections Clostridium difficile colitis.
Drug interactions: Many antimicrobial agents interact with other drugs to increase or decrease their serum levels and effects, This is frequently the case with the antimicrobial agents that are metabolized and/or affect the cytochrome P450 enzyme system (e.g., rifampin is a powerful inducer, whereas macrolides and azole antifungal agents are inhibitors of cytochrome P450 enzymes).
e. Therapeutic failure: Causes of failure of antimicrobial therapy include:
- Ineffective antimicrobial drug.
- Inappropriate dosage or duration of antimicrobial therapy.
- Development of microbial resistance.
- Change of causative pathogens.
4. Route of administration
The route administration of the drugs is determined by the site and severity of the infection, For example, mild and a small area of skin infection can be treated by short-term topical antibiotic preparations. Choice of oral or intravenous therapy will depend on the extent of absorption from the gastrointestinal tract, e.g., ciprofloxacin has good bioavailability when taken orally, and results similar blood levels compared with intravenous administration. Parenteral administration may be required for severe life-threatening infections, or when the oral formulations are not available.
5. Cost
Very often, several drugs show similar efficacy in treating an infection, but they may vary greatly in cost, and they may vary greatly in cost, Sometimes, there are many fold differences in the price of different brands of the same drug, thus, the cost of therapy may be taken into account after accessing the socioeconomic status of the patient, before making the final decision.
Factors related to patient
1. Immune System
The functional state of the host defense mechanism is a critical determinant of the therapeutic effectiveness of the antimicrobial, Both humoral and cellular immunity are important, Immunity of a patient is needed for the final eradication of an infection; yet
a. Bacteriostatic agents are successful in the treatment of infections in immunocompetent hosts.
b. Bactericidal agents are preferred for the treatment of infections in the following conditions:
- Patients with impaired defense mechanisms, eg., AIDs patients, neutropenic patients, and patients receiving immuno-suppressant therapy.
- In the case of serious infections, e.g., endocarditis, where phagocytic cells are excluded from the infected vegetation, and bacterial meningitis, where phagocytic cells are ineffective because of lack of opsonins.
2. Renal functions
Impairment of renal functions may lead to the accumulation of those antimicrobials, which are mainly eliminated by the kidneys. This may result into serious adverse reactions if appropriate dose adjustments are not made. Care must be taken in case of using aminoglycosides, vancomycin, or flucytosine in patients with renal impairment because these drugs are exclusively eliminated by the kidneys.
3. Hepatic functions
For drugs that are concentrated, metabolized, or excreted by the liver (e.g. erythromycin, chloramphenicol, metronidazole, tetracyclines) dose must be reduced in patients with hepatic failure or hepatic dysfunction.
4. Age
Hepatic metabolism and renal excretion mechanism are poorly developed in newborn babies, especially in premature infants. Improper adjustment in dose in such cases may lead to serious consequences, e.g., Gray baby syndrome is caused by chloramphenicol. Elderly people are also prone to the toxic effects of those drugs, which are eliminated by hepatic or renal mechanisms, since these mechanisms are less functional as compared to adult age.
Developmental factors are also primary determinants of the type of antimicrobial used. As tetracyclines bind avidly to developing teeth and bones, their use in children may lead to retardation of bone growth, discoloration, or hypoplasia of tooth enamel. Similarly, fluoroquinolones can accumulate in the cartilage of young bones and may retard the growth of cartilage.
5. Local factors
Local factors at the site of action may greatly influence the effectiveness of anti-microbial in curing the disease, Daptomycin, an excellent bactericidal agent against Gram-positive bacteria, is not useful for the treatment of pneumonia (e.g. pneumococcal pneumonia) because it is inactivated by lung surfactant.
Large accumulations of hemoglobin in infected hematomas can bind to penicillin and tetracycline may reduce their activity. The acid pH of abscess cavities results in a marked loss of antibacterial action of aminoglycosides and erythromycin.
Penetration of antibiotics into infected areas like abscess cavities is impaired because vascular supply is reduced. Successful therapy of abscesses usually requires surgical drainage.
Infections to implants either temporary (e.g., urinary catheter, central venous catheter) or permanent (e.g., prosthetic joint, artificial heart valve) are characterized by the formation of biofilms, a structured community bacterial cells enclosed in a self-produced polymeric matrix adherent to an inert or living surface, Bacteria in biofilms are protected against antibacterial therapy, Antibacterial such as fluoroquinolones, rifampin, and ampicillin penetrate well through the matrix.
6. Genetic factors
e.g., patients with severe deficiency glucose-6-phosphate dehydrogenase can develop significant hemolysis when exposed to sulfonamides, nitrofurantoin, and antimalarials.
7. Pregnancy
Antibiotics easily cross the placental barrier and may affect, e.g. hearing loss in children may be associated with aminoglycosides therapy given to the mothers during pregnancy, Tetracyclines administration in pregnant females can affect the growth of bones and teeth of a fetus.
8. Allergy
Allergy precludes the use of allergic antibiotics, It is because the immediate or accelerated reactions caused by the allergic antimicrobials can cause fatal results. Examples penicillin and cephalosporins.
Combinations of antimicrobial drugs
Indications of combinations of antimicrobial drugs:
1. Empiric therapy in critically ill patients.
2. Severe infections, e.g., septic shock with growing Gram-negative bacilli, particularly P. which is both a common nosocomial pathogen and frequently resistant to multiple agents, a combination of an antipseudomonal β-lactam with a fluoroquinolone or an aminoglycoside could be used.
3. Mixed (Polymicrobial) infections: To extend the antimicrobial spectrum, e.g., most intra-abdominal infections are usually caused by multiple organisms with a variety of Gram-positive cocci, Gram-negative bacilli, and anaerobes, Antimicrobial combinations, such as a third-generation cephalosporin or a fluoroquinolone plus metronidazole can be used.
4. To delay the emergence of resistant strains: As in the treatment of tuberculosis, HIV, and hepatitis C virus infections.
5. Synergism: To achieve an effect not obtained by either antimicrobial alone, as one drug enhances the antimicrobial activity of the second drug. e.g., in enterococcal bacterial endocarditis, the combination of penicillin, and aminoglycoside is successful as compared to frequent failure with penicillin alone.
6. To reduce the incidence or intensity of adverse reactions.
Misuse of Antimicrobial Drugs
Causes of Misuse of antimicrobial drugs:
1. Treatment of fever of undetermined origin: Antibiotics may be associated with undefined viral infection or due to other causes, e.g. lymphoma, cancer, metabolic disorders, hepatitis atypical rheumatoid arthritis, etc. Therefore, the cause must be defined.
2. Prolonged empiric antimicrobial treatment without clear evidence of Infection: Continued use of antibiotics, especially broad-spectrum antibiotics, can seriously disrupt the normal ecology of the body and render anyone more susceptible to pathogenic bacteria, yeast, viral, and parasitic infection, i.e., superinfection.
3. Inadequate length of treatment period: antibiotics should be continued until resolution of the infection is achieved. The duration of therapy required varies enormously between different anatomical sites and organisms, It varies from a single dose (e.g., Fosfomycin for treatment of uncomplicated cystitis), days (e.g., 5 days for community-acquired pneumonia, weeks (e.g. 4-6 weeks for endocarditis, osteomyelitis), months (6 months regimen for treatment of drug-susceptible tuberculosis), to years (e.g., regimen for treatment of hepatitis B virus infection), Course of antibiotic, which is shorter than the prescribed one often kills only the most vulnerable bacteria, while allowing relatively resistant bacteria to survive.
4. Inappropriate antimicrobial dosage. If the dosage of the antibiotic is not adequate, it will not be effective for the treatment of the infection and bacteria are more likely to develop resistance.
5. Treatment of a positive clinical culture in the absence of disease, e.g. treatment of asymptomatic bacteriuria in pregnant women.
6. Failure to narrow antimicrobial therapy when a causative organism is identified.
7. Unnecessary prophylactic therapy.
8. Excessive use of certain antimicrobial agents.
9. Reliance on chemotherapy with the omission of surgical drainage of purulent infections (e.g., abscess). Therefore, there should be an antibiotic plus proper drainage.
You can follow science online on Youtube from this link: Science online
You can download Science online application on google Play from this link: Science online Apps on Google Play
Antimicrobial drugs types, use, side effects, resistance & Empiric antimicrobial therapy
Parasitic infections, Immunological tests, DNA probes and Polymerase Chain Reaction
Diagnosis of parasitic infections and Techniques used for identification of Intestinal Parasites
Myiasis classification, diagnosis, causes, treatment & medicolegal importance
Vaccines types, Live vaccines, Inactivated vaccines, Subunit vaccines, Naked DNA & mRNA vaccines