Streptococci symptoms, shape, types, diagnosis and pathogenesis of rheumatic fever
The streptococci are Gram-positive spherical bacteria that characteristically form pairs or chains during growth, They are differentiated from Staphylococci by being catalase-negative, They are widely distributed in nature, Some are members of the normal human flora, and others are associated with important human diseases.
Classification of Streptococci
Streptococci can be classified by their haemolytic activities on blood agar into:
- Alpha (α) Hemolytic streptococci: cause partial destruction of red blood cells. Examples: Viridans streptococci and Streptococcus pneumoniae.
- Beta (β) Hemolytic streptococci that cause complete lysis of the red blood cells in blood agar resulting in a clear zone around the colonies. Those are further grouped on the basis of their cell-wall carbohydrate into serogroups (A-H) and (KU)
- Non-Hemolytic streptococci are unable to hemolyze red blood cells.
Group A β-hemolytic streptococci (streptococcus pyogenes)
The majority of β-hemolytic/streptococci causing infections in man belong to this group of B hemolytic streptococci. It is normally found in the throat or nasal cavity in 5-15% of apparently healthy people (carriers) Like all streptococci, they are Gram-positive cocci, occurring in chains of varying length, non-motile and on sporing.
Cultural characters
In facultative anaerobe, the optimum temperature for growth 37° C. Fastidious i.e. does not grow on nutrient agar. Grows on blood agar. Clear often wide zone of B-hemolysis surrounds colonies on blood agar.
Biochemical activities
Like all streptococci, they are catalase negative. They are sensitive to bacitracin which could be used for its identification in place of antigenic study. Susceptibility to bacitracin is determined by placing a disc saturated with bacitracin onto a plate inoculated with Streptococcus pyogenes, after overnight incubation, the zone of inhibition of growth around the bacitracin disc will be detected.
Antigenic structure
In addition to its carbohydrate (C Ag) group A; Streptococcus pyogenes has and three surface protein antigens (M. T and R) that are useful in serotyping, Of these three, M protein is the most important, M protein acts as a virulence factor by inhibiting phagocytosis, Immunity to infection with group A streptococci is related to the presence of type-specific antibodies to the M protein, Because there are many, perhaps 150 types of M protein, a person can have repeated infections with Streptococcus pyogenes of different M types.
Toxins and enzymes and their role in virulence
- Streptokinase (fibrinolysin): It transforms the plasminogen of human plasma into plasmin, an active proteolytic enzyme that digests fibrin and other proteins, This enzyme works to break up and dissolve blood clots which can block blood vessels, It can be used to lyse thrombi in the coronary arteries of heart attack patients.
- Hyaluronidase (spreading factor): It splits hyaluronic acid, an important component of the ground substance of connective tissue, Thus, hyaluronidase facilitates the rapid spread of Streptococcus pyogenes in skin infections (cellulitis).
- Streptococcal deoxyribonucleases: These enzymes can depolymerize free deoxyribonucleic acid (DNA) present in pus. This process reduces the viscosity of the abscess material and facilitates the spread of the organisms.
- Streptococcal pyrogenic exotoxins: Among these is the classic erythrogenic toxin which is associated with the rash in scarlet fever.
- Haemolysins e.g. Streptolysin O (SLO): It is antigenic and an antibody to streptolysin O develops after infection, Antistreptolysin O (ASO) serum levels higher than 200 Todd are suggestive of recent infection with Streptococcus pyogenes, It also helps in the diagnosis of rheumatic fever.
Pathogenesis and clinical findings
The infections can be divided into several categories:
Pyogenic infections
a. Localized infections
Streptococcal pharyngitis and tonsillitis, Streptococcal pyoderma: local infection of superficial layers of skin, especially in children is called impetigo.
b. Invasive infections
- Erysipelas: If the portal of entry is the skin (through minor cuts or even scratches), erysipelas results, with massive brawny edema and a rapidly advancing margin of infection.
- Cellulitis: Streptococcal cellulitis is an acute, rapidly spreading infection of the skin and subcutaneous tissues, It follows infection associated with mild trauma, burns, wounds, or surgical incisions, Pain, tenderness, swelling, and erythema occur.
- Necrotizing fasciitis (streptococcal gangrene): there is extensive and very rapidly spreading necrosis of the skin, tissues, and fascia, Bacteria enter a wound, such as from an Insect bite, a burn, or a cut.
- Puerperal fever: if the streptococci enter the uterus after delivery, puerperal fever develops, which is essentially septicemia originating in the infected wound (endometritis).
- Bacteremia or sepsis: infection of traumatic or surgical wounds with streptococci results in bacteremia, which can rapidly be fatal, Streptococcus pyogenes bacteremia can also occur with skin infection, such as cellulitis.
Toxin-mediated diseases
- Streptococcal toxic shock syndrome: Fulminant, invasive Streptococcus pyogenes infections with are characterized by shock, bacteremia, respiratory failure and multiorgan failure Death occurs in about 30% of patients. It is usually associated with skin infections, childbirth, trauma and surgeries.
- Scarlet Fever: The classical erythrogenic toxin causes scarlet fever in association with Streptococcus pyogenes pharyngitis) or with skin or soft tissue infection, The rash appears on the trunk after 24 hours of illness and spreads to involve the extremities.
Poststreptococcal diseases (Rheumatic fever, Glomerulonephritis)
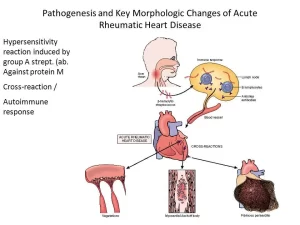
One to four weeks after an acute Streptococcus pyogenes infection, nephritis or rheumatic fever occasionally develops, The latent period suggests that these post-streptococcal diseases are not attributable to the direct effect of disseminated bacteria but instead represent a hypersensitivity response.
Nephritis is more commonly preceded by an infection of the skin; rheumatic fever is more commonly preceded by an infection of the respiratory tract, Rheumatic fever: This is the most serious sequela of Streptococcus pyogenes because it results in damage to heart muscle and valves, Rheumatic fever is more commonly preceded by an infection of the respiratory tract.
There is an antigenic similarity between certain M protein antigens present in certain strains of Streptococcus pyogenes (certain serotypes), and human heart tissue antigens, When patients produce antibodies to these M protein antigens, they cross-react with cardiac tissue antigens, It is an autoimmune disease greatly exacerbated by the recurrence of Streptococcus pyogenes infection.
Laboratory diagnosis of streptococci
Specimens: depend on the nature of the streptococcal infection.
- Throat swab in case of tonsillitis.
- Pus from a skin lesion and wound infection.
- Blood for blood culture in case of bacteremia and sepsis.
- The serum is obtained for antibody determination.
1. Smears
Gram-stained smears of throat swabs are rarely of value in streptococcal pharyngitis because viridians streptococci are part of the normal oropharyngeal flora and cannot be distinguished from the pathogenic Streptococcus pyogenes.
2. Culture
Specimens are inoculated onto blood agar plates and incubated at 37°C. After 24 hours of incubation, plates are examined for β-hemolytic translucent pin-point colonies. Anaerobic Incubation improves haemolysis
Identification
A. Bacitracin sensitivity: Group A streptococci, can be differentiated from the other groups by being sensitive to bacitracin. This is tested for by placing a filter paper disc impregnated with bacitracin on the surface of the culture plate after inoculating it with the organism. A zone of inhibition of growth occurs around the disc if the organism is group A
B. Serological grouping: by using antisera against group antigens.
C. Serotyping: can be made for epidemiological purposes using specific antisera against M and T protein antigens.
3. Antizen detection tests
Several commercial kits (enzyme immunoassay or latex agglutination tests) are available for rapid detection of group A streptococcal antigen from throat swabs, These tests are rapid, inexpensive and specific but the sensitivity of the tests is low, All negative results must be confirmed by a throat culture.
4. Antibody detection (For diagnosis of rheumatic fever)
The measurement of antibodies against streptolysin O (ASO test) is useful for confirming rheumatic fever, These antibodies appear 3 to 4 weeks after the initial exposure to the organism and then persist, the patient’s serum is examined for an elevated antistreptolysin O (ASO titer), A titer of 200 Todd units or more is significant.
Immunity
Resistance against streptococcal diseases is M-type specific, Thus, a host who has recovered from infection by one group A. streptococcal M type is relatively immune to re-infection by the same type but fully susceptible to infection by another M type, Antibody to streptolysin O develops after infection. It blocks hemolysis by streptolysin O but does not indicate immunity, High titers (>200 Todd units) indicate recent or repeated infection and are found more often in rheumatic individuals than in those with uncomplicated streptococcal infections.
Treatment
All Streptococcus pyogenes are susceptible to penicillin G. Macrolides (such as erythromycin) and clindamycin have often been recommended for penicillin-allergic patients, Antimicrobial drugs have no effect on established glomerulonephritis and rheumatic fever, In acute streptococcal infections, however, every effort must be made to rapidly eradicate streptococci from the patient, eliminate the antigenic stimulus and thus prevent post-streptococcal disease.
You can follow Science online on YouTube from this link: Science online
You can download Science online application on Google Play from this link: Science online Apps on Google Play
Control of Drug Resistance & Bacterial resistance to chemotherapeutic agents
Features and classification of viruses, Defective viruses & Viral vectors used for gene therapy
Staphylococci definition, diagnosis of staphylococcal infections & treatment
Antibacterial agents types, Effect of Antibacterial Drugs & How do antibiotics work?
Microbiology, Bacteria structure, types, Gram-positive bacteria & Gram-negative bacteria