Factors determining the arterial blood pressure and coronary circulation
Systolic BP is the maximum pressure exerted in the arteries when blood is ejected into them during systole (range 100-140 mm Hg). Diastolic BP is the minimum pressure within the arteries when blood is draining off into the remainder of the vessels during diastole (range 60-90 mm Hg). The arterial BP is conventionally written as systolic pressure over diastolic pressure eg. 120/80 mm Hg.
Arterial blood pressure
The pulse pressure is the difference between the systolic and diastolic pressures (systolic pressure-diastolic pressure), normally about 40 mmHg. Blood pressure (BP) is the force exerted by the blood against a vessel wall. The mean arterial pressure (MAP) is the average pressure throughout the cardiac cycle (normally about 93 mm Hg).
As systole is shorter than diastole, the mean pressure is slightly less than the value halfway between systolic and diastolic pressure. An approximation to MAP can be obtained by applying the following equation:
Mean arterial pressure = diastolic pressure + 1/3 (pulse pressure)
Blood pressure variability
Blood pressure in the brachial artery in a young adult in the sitting or lying position at rest is approximately 120/80 mm Hg. Blood pressure is a variable that is influenced by many different factors, including:
- Age: Both systolic and diastolic BP rise with advancing age. However, after middle age, systolic BP continues to rise, while diastolic BP starts to decrease due to increased stiffness of the arteries. Consequently, the pulse pressure is increased.
- Sex: BP is lower in young women than young men until age 55-65, after which they become comparable.
- Anxiety: anxiety raises BP, especially systolic (due to increased sympathetic stimulation), often by as much as 30 mm Hg. This is usually reduced with reassurance and familiarization with the technique of BP measurement. “White coat hypertension” is a condition in which a subject with a normal BP becomes hypertensive during BP measurement, but pressures then settle to normal outside the medical environment.
- Circadian variation: BP normally falls up to 20 mm Hg during sleep. This fall is reduced or absent in hypertension. Consequently, normal people are sometimes called “dippers” and hypertensives “non-dippers”.
- Exercise: systolic BP increases markedly during exercise; the diastolic BP does not change or even decreases by endurance exercise.
- Obesity: there is an association between obesity and hypertension. However, BP may be overestimated if a small cuff was used in the measurement of BP (cuff hypertension).
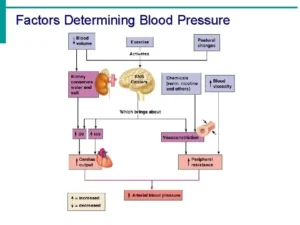
Factors determining the arterial blood pressure
Arterial pressure (ΔP) = Cardiac output (Q) x Peripheral resistance (R).
Arterial BP acts as the driving force for blood flow through the tissues of the body. For blood to flow through a vascular bed there must be a pressure gradient between the arterial and venous ends of this bed. The size of that gradient (ΔP) equals the rate of blood flow (F) times the resistance to flow (R) i.e. ΔP = F x R (note that this is a rearrangement of the basic flow equation).
Applying this to the systemic circulation, ΔP is the pressure gradient between the aorta and the right atrium. Since atrial pressure is close to zero, ΔP is equal to the arterial BP. The total blood flow through the systemic circulation is the cardiac output. This is an important relationship because it indicates that BP may be regulated through changes in either cardiac output or peripheral resistance.
(1) Cardiac output:
The arterial BP is directly proportional to the cardiac output, which is equal to stroke volume x heart rate.
- Effect of changes in stroke volume: an increase in the stroke volume raises mainly the systolic BP with no significant change in diastolic BP
- Effect of changes in heart rate; an increase in heart rate raises mainly the diastolic BP due to shortening of the diastolic period (which prevents fall of the diastolic pressure to the normal level).
(2) The peripheral resistance
It is the total resistance to blood flow through the systemic circulation. The peripheral resistance is essential for the maintenance of arterial BP particularly the diastolic. It is produced mainly in the arterioles and is determined by the radius of the vessel, blood viscosity, and length of the vessel. Normally, adjusting the arteriolar diameter can modify it, because the other 2 factors are normally kept constant.
Regulation of the arterial blood pressure
(A) Short-term mechanisms (nervous):
These are potent rapidly acting pressure control mechanisms. They start acting within few seconds after the alteration of the BP, and their action lasts for several hours then declines. They are mostly nervous reflexes. They include the following:
- Arterial baroreceptor reflexes (pressure buffer system)
- Atrial stretch receptor reflexes
- Peripheral chemoreceptor reflexes
- Cushing’s reflex (or reaction)
- The central nervous system (CNS) ischemic response
(These reflexes are discussed before in the cardiovascular regulatory mechanisms)
(B) Intermediate-term mechanisms
These mechanisms control the arterial BP by adjusting the vascular capacity and resistance as well as the blood volume. They start acting within few minutes after the alteration of the BP and their action lasts for several days then declines. During this time, the nervous (rapid) mechanisms usually fatigue and become less and less effective. Such intermediate-term control mechanisms include the following:
1. Capillary fluid shift mechanism
This mechanism occurs especially when the arterial BP is altered as a result of changes in the blood volume. An increase in the blood volume increases the capillary hydrostatic pressure, and this helps fluid filtration into the tissue spaces, thus the blood volume is decreased, leading to a reduction of the arterial BP toward the normal level. The opposite occurs when the blood volume is decreased.
2. Hormonal regulation
This mechanism regulates the arteriolar diameter and peripheral resistance. It includes Catecholamine, vasopressin, and the renin-angiotensin system, which are previously discussed in systemic regulation of the arteriolar diameter.
(C) Long-term mechanisms: “control urine output”
These mechanisms control the arterial BP by the renal-body fluid mechanism (i.e. by adjusting the body fluids and blood volumes through modifying the excretion of water and salt by the kidneys. This occurs by variation of the glomerular filtration rate and secretion of the aldosterone hormone.
The coronary circulation
Coronary blood flow
- The resting coronary blood flow in the human being averages about 250 ml/min (5% of the total cardiac output).
- During exercise, the coronary blood flow increases 3-4 folds.
- The capillary blood flow in the left ventricle falls to a low value during systole due to the strong compression of the left ventricular muscle around the intramuscular vessels.
- During diastole, the cardiac muscle relaxes and no longer obstructs the blood flow through the left ventricular muscle capillaries, so that blood flows rapidly during all of the diastole.
- The phasic changes in blood flow through the coronary capillaries of the right ventricle are less pronounced due to the far less force of contraction of the right ventricle
Tachycardia shortens the period of diastole; this reduces coronary flow. However, this is overridden by coronary dilation associated with the increased metabolic activity of the heart.
Regulation of coronary blood flow:
A) Autoregulation: metabolic factors:
Blood flow through the coronary system is regulated almost entirely by the vascular response to the local needs of the cardiac muscle for nutrition. Increased cardiac work leads to hypoxia (the most important factor), elevated H+, CO2, K+, lactate, prostaglandins, and adenosine concentrations.
These factors cause coronary vasodilatation, which increases blood flow and O2 supply to the cardiac muscle. Hypoxia is the most effective coronary vasodilator. Hypoxia causes coronary vasodilatation via:
- A direct effect on the coronary vessels.
- The release of adenosine, a vasodilator substance.
B) Neural Factors:
The coronary arterioles contain:
- α-adrenergic receptors, which mediate vasoconstriction.
- β-adrenergic receptors, which mediate vasodilatation.
When the inotropic and chronotropic effects of sympathetic discharge are blocked by a beta-adrenergic blocking drug, stimulation of the sympathetic nerves causes coronary vasoconstriction. Thus, the direct effect of sympathetic stimulation to the coronary vessels is constriction rather than the dilation of the coronary vessels.
However, sympathetic stimulation causes coronary vasodilatation secondary to increased cardiac work and production of vasodilator metabolites (metabolic autoregulation), which overrides the direct vasoconstrictor α-adrenergic effect. Vagus nerve stimulation slightly dilates the coronary vessels.
When the mean arterial blood pressure falls, the overall effect of the reflex increase in sympathetic discharge is increased coronary blood flow secondary to the metabolic changes in the myocardium at a time when the cutaneous, renal, and splanchnic vessels are constricted, In this way, the circulation of the heart, like that of the brain, is preserved when flow to other organs is compromised, Therefore, coronary blood flow is predominantly under non-neural control.
FAQ About Factors Determining Arterial Blood Pressure and Coronary Circulation
What are the main factors that determine arterial blood pressure?
Arterial blood pressure is mainly determined by:
- Cardiac output (amount of blood pumped by the heart per minute).
- Peripheral resistance (narrowing or widening of blood vessels).
- Blood volume.
- Blood viscosity (thickness of blood).
- Elasticity of arterial walls.
How does cardiac output affect arterial blood pressure?
When the heart pumps more blood per minute (increased cardiac output), arterial blood pressure rises. When cardiac output decreases, blood pressure falls.
What is the role of peripheral resistance in controlling blood pressure?
Peripheral resistance depends on the diameter of blood vessels:
- Vasoconstriction (narrow vessels) → increases blood pressure.
- Vasodilation (wide vessels) → decreases blood pressure.
How does blood volume influence arterial blood pressure?
An increase in blood volume raises blood pressure because more blood presses against the vessel walls. A decrease in blood volume lowers blood pressure, as seen in dehydration or blood loss.
Does blood viscosity affect arterial blood pressure?
Yes. Thick blood (high viscosity) increases resistance to flow and raises blood pressure.
Thin blood flows more easily and lowers resistance.
What is the effect of arterial elasticity on blood pressure?
Elastic arteries expand easily and help maintain normal pressure. Stiff or less elastic arteries (as in aging or atherosclerosis) cause higher blood pressure.
What is coronary circulation?
Coronary circulation is the blood flow that supplies oxygen and nutrients to the heart muscle (myocardium) through the coronary arteries.
Why is coronary circulation important?
The heart needs a constant oxygen supply to pump blood. Poor coronary circulation can lead to:
- Chest pain (angina).
- Heart attack (myocardial infarction).
- Heart failure.
What factors determine coronary blood flow?
Coronary circulation is affected by:
- Heart muscle metabolism (oxygen demand).
- Diameter of coronary arteries.
- Blood pressure in the aorta.
- Duration of diastole (heart relaxation phase).
- Presence of coronary artery disease.
How does heart activity affect coronary circulation?
Coronary blood flow increases during heart relaxation (diastole). During heart contraction (systole), coronary vessels are compressed, reducing blood flow temporarily.
How does atherosclerosis affect coronary circulation?
Atherosclerosis narrows the coronary arteries, reducing blood flow to the heart muscle. This may cause chest pain, shortness of breath, and increase the risk of heart attacks.
Can stress and exercise affect arterial blood pressure and coronary circulation?
Yes. Stress increases heart rate and blood pressure. Exercise temporarily raises blood pressure but improves coronary circulation and heart health in the long term.
What hormones regulate arterial blood pressure?
Important hormones include:
- Adrenaline (epinephrine).
- Renin–angiotensin–aldosterone system (RAAS).
- Antidiuretic hormone (ADH).
- Nitric oxide (vasodilator).
What happens when coronary circulation is reduced?
Reduced coronary blood flow leads to insufficient oxygen supply to the heart muscle, causing:
- Fatigue.
- Chest pain.
- Risk of myocardial infarction.
How can arterial blood pressure and coronary circulation be kept healthy?
You can protect both by:
- Regular physical activity.
- Healthy diet (low salt and saturated fat).
- Avoiding smoking.
- Managing stress.
- Regular blood pressure and heart checkups.
You can follow Science Online on YouTube from this link: Science Online
Regulation of blood flow, Renin-angiotensin vasoconstrictor system and Vasodilator hormones
Physiology of the circulatory system & How does the circulatory system work
Blood vessels structure, function, layers, characteristics, and How blood vessels work
Anatomy of the circulatory system, Vascular system, Arteries of head and neck