Cyanosis, Hypoxia types, causes, symptoms and Effectiveness of O2 therapy in treatment of hypoxia
Hypoxia can affect the whole body, or affect a region of the body, hypoxia symptoms are shortness of breath while resting, severe shortness of breath after physical activity, decreased tolerance to physical activity, waking up out of breath, feelings of choking, wheezing, frequent cough, and bluish discoloration of the skin.
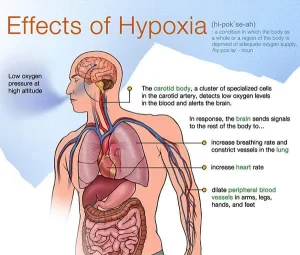
Hypoxia
Hypoxia is an O2 deficiency at the tissue level. It can lead to hypercapnia, which takes place when the lungs retain too much carbon dioxide due to breathing difficulties. However, hypoxia is a pathological condition, variations in arterial oxygen concentrations can be part of normal physiology, for example, during hypoventilation training or strenuous physical exercise.
Types of hypoxia
- Hypoemxic hypoxia.
- Anemic hypoxia.
- Stagnant hypoxia.
- Histotoxic hypoxia.
Hypoxomic hypoxia
A condition in which PaO2 is decreased in arterial blood i.e. Hb is not fully saturated (O2 content is decreased).
Causes:
- Decreased partial pressure of O2 in inspired air at sea level or high altitude.
- Intracardiac shunt (right to left shunt) as in atrial septal defect or ventricular septal defect.
- Pulmonary diseases as:
a. Hypoventilation which may be due to: RC depression by drugs as morphine or paralysis of the respiratory muscles.
b. Diffusion defect:
- Interstitial pulmonary fibrosis (thickening of respiratory membrane → decreased diffusion leading to decrease PaO2 in arterial blood).
- Emphysema: there is inadequate perfusion to the well-ventilated alveoli and good perfusion to the poorly ventilated alveoli.
c. Intrapulmonary right to left shunt:
- Reversible shunt: occurring in normal vessels that perfuse regions of the lung that are not ventilated at all e.g. in pneumonia, atelactasis → collapse of the lung alveoli → bad ventilation.
- Irreversible shunt: as in pulmonary arteriovenous fistula.
d. V/Q mismatch.
Anaemic hypoxia
In which PaO2 is normal but there is a reduced amount of Hb that carries O2 (O2 content is decreased).
Causes:
- Anaemia: where the decrease in Hb may be due to deficiency of the essential nutrients as iron. At rest, hypoxia due to anemia is not severe unless Hb deficiency is marked because it is compensated by increased 2-3 DPG. During exercise, the hypoxic effect may be severe because of the limited ability to increase O2 delivery to the active tissues.
- CO poisoning: CO reacts with Hb to form carboxyhemoglobin which is a non-functioning Hb. It shifts O2-Hb dissociation curve of the remaining oxyheamoglobin to the left thus increases the affinity of Hb to O2 and decreases O2 released to tissues.
Stagnant hypoxia
A condition in which the blood flow to the tissues is slow or stagnant i.e. inadequate to the tissues. The amount of O2 delivered to the tissues is inadequate inspite of normal PaO2 and normal Hb. The slow blood flow increases the withdrawal of O2 from blood in capillaries. Therefore, O2 content in venous blood is markedly reduced.
Histotoxic hypoxia
A condition in which an adequate amount of O2 is delivered to tissues but the tissues become unable to utilize O2 due to the presence of a toxic substance (eg cyanide). PaO2 and O2 content are normal. Cyanide blocks the action of cytochrome oxidase, thus cannot utilize O2.
Treatment of cyanide poisoning: Injection of mythelene blue or nitrite. They form metHb which has the ability to attract cyanide and bind with it forming nontoxic cyanmetHb. It is then removed from the circulation via the liver or kidney.
Effects of hypoxia
There is an increase in the rate of ventilation which is proportional to the severity of hypoxia on the peripheral chemoreceptors.
- In moderate hypoxia: As the brain is most affected by hypoxia than other organs, hypoxia usually leads to mental aberration, impaired judgment, drowsiness, excitement, disorientation, loss of time sense, and headache. Also, it may affect other organs causing anorexia, nausea, vomiting, tachycardia, and hypertension.
- In severe hypoxia: If the PO2 is less than 20 mmHg, it affects the brain causing loss of consciousness in about 20 seconds.
Effectiveness of O2 therapy in the treatment of hypoxia
- In hypoxemic hypoxia: It is of great importance because it increases PO2 in inspired air (except in right to left shunt).
- In anemic hypoxia, It is of no value because the defect is in Hb.
- In stagnant hypoxia, It is of no value because the problem is in the slow blood flow.
- In histotoxic hypoxia, It is of no value because O2 cannot be utilized by the cells.
Cyanosis
It is a bluish discoloration of the skin and mucous membrane due to an abnormal increase in the amount of reduced Hb in the blood.
Cyanosis is not liable to occur in:
- Anemic hypoxia: The total amount of Hb in the blood is decreased, thus the concentration of reduced Hb will never reach the threshold cyanosis.
- CO poisoning: The colour of HbCO is cherry red. HbO2 in the presence of HbCO is difficult to be reduced.
- Histotoxic hypoxia: The amount of HbO2 is increased in both arterial and venous blood and the reduced Hb is very little because the tissues cannot use O2.
You can follow Science Online on YouTube from this link: Science online
Acute hypercapnia, Non-chemical modulation of ventilation and ventilation response to exercise
Central and Chemical regulation of ventilation, Central and Peripheral chemoreceptors
Carbon dioxide transport from tissues to lungs, Tidal CO2 and Haldane effect
Oxygen transport by blood, Importance of P50, Bohr Effect and Treatment of CO poisoning
Ventilation-perfusion relationships and why is ventilation higher at the base of the lung
Regional differences in ventilation, Pulmonary circulation, Shunt and Lung perfusion zones