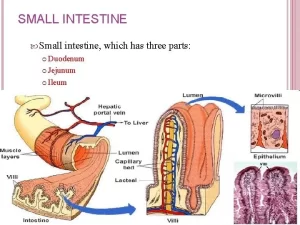
Small intestine constituents, Regulation, function and Digestion in the small intestine
The small intestine is the longest part of the GI tract, and it is where most of your digestion takes place, When food leaves your stomach, it enters the small intestine, It is also called the small bowel, The small bowel connects to the large bowel, also called the large intestine or colon, The intestines are responsible for breaking food down, absorbing its nutrients and solidifying the waste.
Physiology of the small intestine
In the living human, the distance between the pylorus and the ileocecal valve is about 280 cm. After death it loses its tone and elongates to more than double its length during life, The first portion of the duodenum is called “duodenal cap” or “bulb”, it is the region which is mostly affected by gastric acid secretion passed through the pylorus, and is a common site for duodenal ulceration.
The small intestine performs both endocrine functions by secretion of hormones and exocrine functions by secretion of digestive enzymes. In the lumen of the small intestine, the intestinal contents are mixed with the secretions of the mucosal cells and with pancreatic secretion and bile, The intestinal secretion is also called succus entericus, The intestinal secretion is made up of mucus and digestive juice.
Constituents of the intestinal secretion
A- Mucus
It is secreted from:
1- Brunner’s glands: These are present in the first few cm of the duodenum only. Brunner’s glands secrete thick alkaline mucus to protect the duodenum from the highly acidic, gastric chyme that enters into it. Brunner’s glands secretion is stimulated by:
- Contact of acidic chyme with duodenal mucosa.
- Vagal stimulation.
- Secretin hormone.
Their secretion is inhibited by sympathetic stimulation (leaving the first part of duodenum unprotected and liable to duodenal ulceration.).
2. Goblet cells: Goblet cells are scattered all over the mucosal surface of the small intestine, They secrete mucus in response to mechanical or chemical stimulation by food.
3. Mucus cells in the intestinal glands “crypts of Lieberkuhn”, This secretion is controlled by local nerve plexuses.
B – Digestive Juice
It is secreted from the intestinal glands (crypts of Lieberkuhn), About one liter is secreted daily, Pure intestinal juice is similar to extracellular fluid with a pH of 7-7.5 and contains no digestive enzymes, The intestine supplies a fluid environment in which the processes of digestion and absorption can occur, The rapid reabsorption of the intestinal juice by the villi provides a water vehicle for absorption of nutrients, The free surface of the epithelial cells of the villi are divided into minute microvilli which form a brush border.
Digestion in the small intestine
The final digestion in the intestine occurs in three locations: the intestinal lumen, the brush border, and the cytoplasm of the mucosal cells.
- The digestive enzymes are present in the brush border of the mucous cells of the intestinal villi, The intestinal digestion mainly occurs at this brush border (membrane or brush border digestion).
- Intestinal cells when desquamated, their enzymes are mixed with the intestinal juice, In this way, about 30 gm of cellular enzymes and proteins are secreted in succus entericus daily (luminal digestion), The cast of cells are replaced by regeneration of new cells from the deep parts of the glands. The life span of an intestinal mucosal cell is 3-5 days.
- Lastly, intracellular or cytoplasmic digestion by the enzymes located in the cytoplasm of intestinal mucosal cells.
A- Protein digestion
In the small intestine, the polypeptides formed by digestion in the stomach are further digested by the powerful proteolytic enzymes of the pancreas and intestinal mucosa, such as aminopeptidases, carboxypeptidases, endopeptidases, and dipeptidases in the brush border of the mucosal cells. In addition, Some di- and tripeptides are actively transported into the intestinal cells and hydrolyzed by intracellular peptidases to amino acids.
B- Carbohydrate digestion
The oligosaccharidases and disaccharidases are responsible for the further digestion of carbohydrates are located in the brush border of small intestinal epithelial cells. These are:
- Maltase and isomaltose: split maltose and maltotriose into glucose.
- Sucrase: acts on sucrose, maltose and maltotriose into glucose and fructose.
- Lactase: splits lactose into glucose and galactose.
- Trehalase: hydrolyzes trehalose into two glucose molecules.
Deficiency of one or more of the brush border oligosaccharidases may cause diarrhea, bloating, and flatulence after ingestion of sugar, The diarrhea is due to the increased number of osmotically active oligosaccharide molecules that remain in the intestinal lumen, causing the volume of the intestinal contents to increase.
C- Lipids
Small amounts of intestinal lipase are secreted, It splits neutral fats into monoglycerides and fatty acids.
D. Digestion of nucleic acids
Nucleases split nucleic acids to pentoses, purine, and pyrimidine base.
Regulation of intestinal secretion
I- Nervous control
a) Through local enteric reflexes: Contact with food, chemical stimulation of mucosal cells or distension of the small intestine initiates local enteric reflex (in the submucosal plexus) resulting in secretion of succus entericus from the crypts of Lieberkuhn.
b) Vagal stimulation stimulates secretion of mucus from Brunner’s glands only, The most important regulatory mechanism is by various local nervous reflexes.
II- Hormonal control
Intestinal secretion is stimulated by the vasoactive intestinal peptide (VIP), secretin and CCK.
- a) Vasoactive intestinal peptide (VIP) is found in nerves in the gastro-intestinal tract and thus is not itself a hormone but a neurotransmitter or a co-transmitter, It is also found in the brain and many autonomic nerves, It markedly stimulates intestinal secretion of electrolytes and hence of water. In addition, it causes relaxation of gastrointestinal smooth muscles, including sphincters; dilation of peripheral blood vessels; and inhibition of gastric acid secretion. It potentiates the action of acetylcholine in salivary glands.
- b) Secretin and CCK.
Small intestine function, anatomy, parts, Arterial supply of the duodenum, midgut & hindgut
Histological structure of stomach, Fundic glands of Stomach & Gastric musculosa
Abdomen muscles, Blood Supply of Anterior Abdominal Wall & Rectus Sheath content
Large Intestine function, parts, length, anatomy & Relations of the rectum
Pancreatic secretion composition, regulation, function, Differences between jejunum & ileum